If you have chronic kidney disease, or even just abnormal kidney lab results, it is normal to wonder whether your primary care doctor is enough or whether it is time to see a nephrologist, a doctor who specializes in kidney disease. The answer is not the same for everyone. Some people with early CKD are monitored in primary care for quite a while, while others need specialist input sooner because their kidney numbers are dropping, their symptoms are worsening, or the cause of the kidney problem is not clear.
For many people in Angleton and Brazoria County, the better question is not “Do all CKD patients need a nephrologist?” but rather “What signs usually mean it is time to involve one?” That is the question this article answers. The decision usually depends on a mix of eGFR, urine albumin results, symptom burden, complication risk, how quickly kidney function is changing, and whether the diagnosis is straightforward or more complex.
Medical disclaimer: This article is for educational purposes only. It is not medical advice, diagnosis, or a substitute for care from a licensed healthcare professional.
What a nephrologist does
A nephrologist is a kidney specialist. They help diagnose and manage kidney disease, evaluate why kidney function is changing, manage CKD complications, adjust medicines for kidney safety, and help plan for advanced treatment if kidney failure becomes a concern. NIDDK’s CKD management guidance explains that nephrology involvement becomes especially useful when the case is no longer routine or when treatment becomes more complex.
That does not mean every person with CKD needs a nephrologist immediately. NIDDK states that, except for very advanced CKD, many of the main treatment steps overlap with good diabetes and cardiovascular care and can often be handled by a primary provider working over time with the patient. It also notes that referral timing varies depending on the patient’s condition and the provider’s experience.
So the role of nephrology is not to replace all other care. It is to add kidney-specific expertise when the situation becomes more serious, more uncertain, or harder to manage well in routine follow-up.
The biggest signs it may be time to see a nephrologist
One of the clearest signs is an eGFR below 30 mL/min/1.73 m². NIDDK’s professional CKD guidance says nephrology involvement is especially important to help prepare for kidney replacement therapy when eGFR is under 30, and National Kidney Foundation identifies stage 4 CKD as severe loss of kidney function, with an eGFR of 15 to 29.
Another major sign is that your kidney numbers are dropping quickly. NIDDK specifically says nephrology consultation may be appropriate to assess rapid decrease of eGFR. This matters because a steadily falling eGFR can mean the kidneys are under ongoing stress and the cause, speed, and treatment plan may need closer review than routine monitoring alone.
A third sign is persistent or worsening albumin in the urine. NIDDK explains that albuminuria is a sign of kidney disease, is important for monitoring progression, and helps guide treatment decisions. When protein leakage in the urine remains significant or keeps worsening, that often strengthens the case for asking whether specialist care is needed.
A fourth sign is that the cause of kidney disease is still not clear. NIDDK says nephrologists may help with a diagnostic challenge, including questions such as whether a biopsy or deeper workup is needed. If the pattern of CKD does not fit the usual picture of diabetes- or blood-pressure-related kidney disease, specialist evaluation becomes more important.
CKD complications that often justify nephrology follow-up
Referral is not only about stage. Some people need nephrology because CKD complications are becoming harder to manage. NIDDK specifically lists blood pressure problems, anemia, mineral and bone disorders, hyperkalemia, hyperphosphatemia, secondary hyperparathyroidism, and malnutrition as therapeutic challenges where nephrology input may be appropriate.
That means nephrology may be worth discussing even before stage 4 if you have difficult-to-control blood pressure, repeated high potassium, CKD-related anemia, worsening bone and mineral issues, or other lab abnormalities that keep coming back despite treatment. In other words, the need for referral is sometimes driven by complexity, not just by one kidney number.
This is especially important because CKD complications do not stay neatly separated from the kidneys. High potassium can affect the heart. Anemia can worsen fatigue and weakness. Mineral and bone problems can affect bones and blood vessels. When these issues are becoming part of the day-to-day picture, kidney-specific management often helps.
Kidney disease causes that should raise the referral question sooner
Some types of kidney disease deserve earlier specialty involvement because they are not simple “watch and wait” cases. NIDDK specifically says nephrologists help treat most primary kidney diseases, including glomerulonephritis.
So if there is concern for a primary kidney disease, unexplained blood or heavy protein in the urine, unusual inflammation-related findings, or a structural or inherited kidney problem, the referral question should come up sooner rather than later. These cases often require more specialized evaluation than ordinary CKD follow-up.
The same applies if there is a strong family history, recurrent unexplained abnormalities on urine testing, or kidney findings that do not match the more common patterns seen with diabetes and hypertension. Those are the situations where “we should probably look deeper” becomes a reasonable next step.
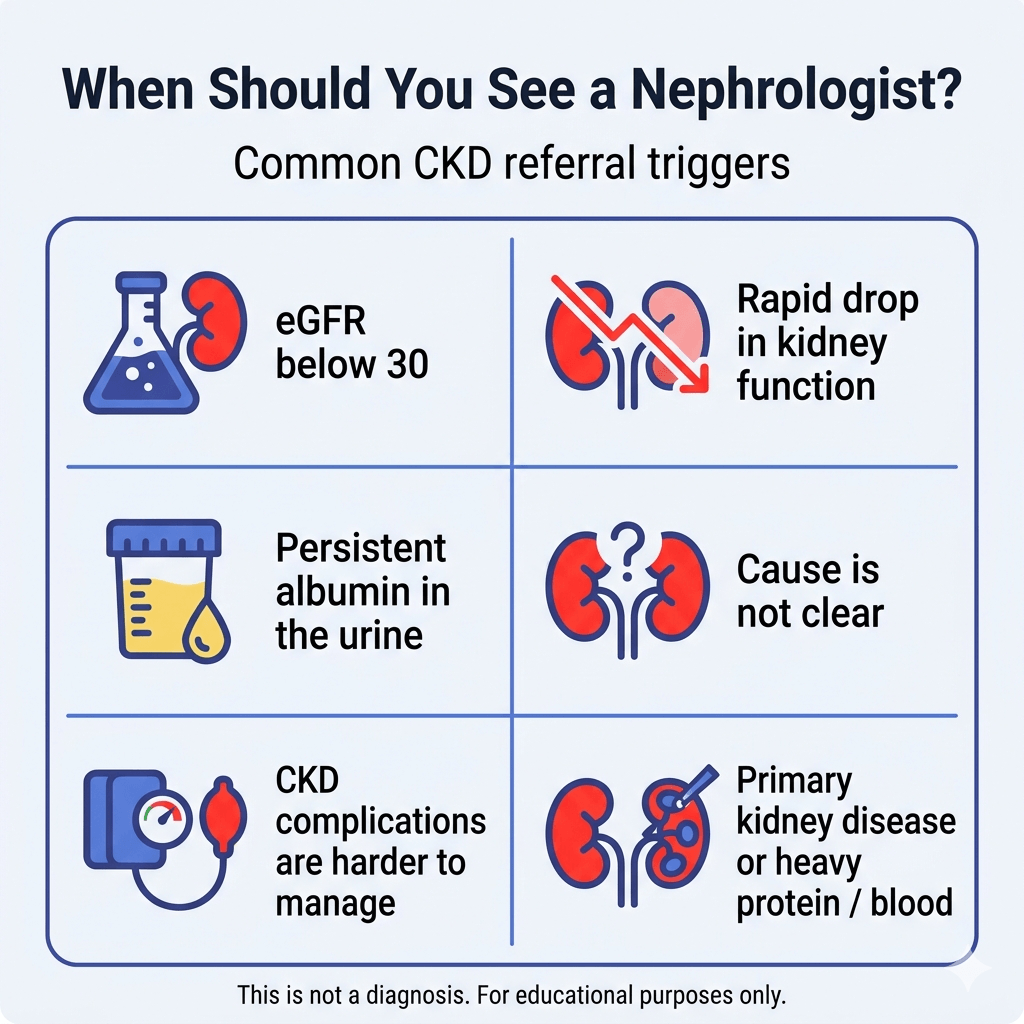
Stage-based guidance: when referral becomes more likely
In stage 1 and stage 2 CKD, many patients are still mainly managed in primary care, especially if the cause is known, blood pressure is controlled, and kidney function is stable. NIDDK’s diagnosis page notes that a GFR under 60 may mean kidney disease, but it does not mean every person at that level automatically needs urgent specialty care.
In stage 3 CKD, referral becomes more of a judgment call. Some people remain stable and continue with primary care monitoring, while others need nephrology because of progression, complications, or uncertainty about the diagnosis. This is where trends over time become more important than one isolated lab result.
In stage 4 CKD, specialist involvement becomes much more important. NKF’s stage 4 patient guidance specifically includes the question, “Can you refer me to a nephrologist (kidney specialist)?” among the key discussion points for this stage, and NIDDK’s professional guidance highlights referral preparation when eGFR is below 30.
In stage 5 CKD, nephrology care is generally central because treatment planning becomes much more urgent and kidney replacement therapy may need to be discussed or underway. NKF and NIDDK both define kidney failure at an eGFR of less than 15.
Symptoms that should make someone ask sooner
Symptoms do not replace lab testing, but they do matter. If CKD is accompanied by swelling, nausea, vomiting, fatigue, worsening weakness, trouble breathing, or major urine changes, it is reasonable to ask whether the current level of care is enough or whether kidney-specialist follow-up should happen sooner. NKF lists these among the common symptoms that become more noticeable in advanced CKD, especially stage 4.
The reason symptoms matter is simple: they may reflect fluid buildup, worsening toxin buildup, anemia, metabolic imbalance, or a faster decline than the lab trend alone suggests. Symptoms do not prove that nephrology is required immediately, but they are part of the decision-making picture.
This is even more important if symptoms are paired with diabetes, long-standing high blood pressure, known albuminuria, or a recent drop in eGFR. When multiple risk signals line up at once, it is safer to ask the referral question earlier.
What a nephrologist may do that is different from routine follow-up
A nephrologist may look more closely at why CKD is happening, not just whether it is present. That can include reviewing the pattern of kidney decline, the degree of albuminuria, whether imaging or serology is needed, or whether a biopsy should even be considered. NIDDK specifically includes diagnostic challenges among reasons to consult nephrology.
They may also help with medication safety and complication management. In CKD, medicine dosing can change, some drugs become riskier, and lab abnormalities like high potassium or acidosis may need tighter kidney-specific management. NIDDK identifies these treatment problems as one of the clearest reasons nephrology input becomes helpful.
And if kidney function is reaching the stage where future dialysis or transplant decisions may eventually matter, nephrology can help patients prepare early rather than late. NIDDK specifically notes that this is especially important when eGFR is below 30.
Questions to ask if nephrology referral may be needed
A good way to make this more practical is to ask your current care team a few direct questions:
- What are my current eGFR and uACR numbers?
- Are my kidney numbers stable or falling?
- Do I have CKD complications that are becoming harder to manage?
- Is the cause of my kidney disease clear?
- Would nephrology help now, or is it reasonable to monitor first?
These questions matter because CKD decisions are rarely made on symptoms alone. NIDDK’s CKD testing guidance centers the discussion on GFR and urine albumin, and NKF’s stage 4 guidance emphasizes talking about the next steps in monitoring, medication safety, complications, and referral.
When symptoms or lab changes should not wait
Some situations should not sit until a routine referral visit. A rapid drop in kidney function, severe swelling, worsening shortness of breath, repeated vomiting, confusion, very low urine output, or fast-worsening weakness can signal a more urgent problem. NIDDK highlights rapid eGFR decline as a reason to involve nephrology, and NKF’s advanced-stage CKD guidance describes many of these symptoms as signs of more serious disease burden.
This does not mean every symptom automatically requires emergency care, but it does mean that some changes should be treated as more than routine CKD follow-up. If symptoms are accelerating or the person is clearly deteriorating, it is safer to seek urgent evaluation instead of waiting weeks for an ordinary appointment.
For people in Angleton and Brazoria County, this is often the hardest part: knowing when CKD is progressing quietly and when it has crossed into something more urgent. If swelling, vomiting, weakness, confusion, breathing problems, or a sharp change in urine output is happening, Angleton ER can help evaluate urgent symptoms and determine what kind of kidney follow-up is needed next.
Frequently Asked Questions
What does a nephrologist do for CKD?
A nephrologist evaluates and treats kidney disease, helps identify the cause, manages CKD complications, adjusts medicines for kidney safety, and helps plan for advanced treatment when needed.
Does everyone with CKD need a nephrologist?
No. NIDDK says many CKD patients, especially outside very advanced disease, can be managed in primary care, with referral timing varying by the patient’s status and the provider’s experience.
At what eGFR should you see a nephrologist?
A common trigger is eGFR below 30 mL/min/1.73 m², because this is where stage 4 begins and referral becomes especially important for planning and complication management.
Should someone with stage 3 CKD see a nephrologist?
Sometimes. It depends on progression, symptoms, albuminuria, complications, and whether the diagnosis is straightforward or uncertain.
Why is stage 4 CKD different when it comes to referral?
Because stage 4 means severe loss of kidney function, with eGFR 15 to 29, and this is where risk of kidney failure and CKD complications becomes much higher.
Can primary care manage CKD without nephrology?
Yes, in many earlier or stable cases. But nephrology becomes more useful when the case is advanced, fast-changing, or harder to manage.
What symptoms should make me ask for referral sooner?
Swelling, worsening fatigue, nausea, vomiting, shortness of breath, major urine changes, or other signs that CKD symptoms are becoming more noticeable.
Can a nephrologist help slow kidney disease progression?
They may help by clarifying the diagnosis, managing complications, adjusting treatment, and planning earlier when risk is increasing. That is an inference based on the reasons NIDDK gives for nephrology consultation.
What tests matter most before referral?
The two most important routine CKD tests are eGFR and urine albumin testing, because they help show kidney function and kidney damage.
When should CKD symptoms be treated urgently instead of waiting?
When there is rapid deterioration, severe swelling, trouble breathing, persistent vomiting, confusion, very low urine output, or a fast overall decline.

