If you’re googling what is coronary heart disease, you’re probably not looking for a textbook definition. You want to know:
- What it actually means (in real life, not medical jargon)
- What it can feel like
- What causes it
- How we check for it
- What you can do about it
- And what symptoms are warning symptoms that shouldn’t wait
Let’s walk through it the same way I’d explain it to a patient sitting in front of me.
Coronary heart disease
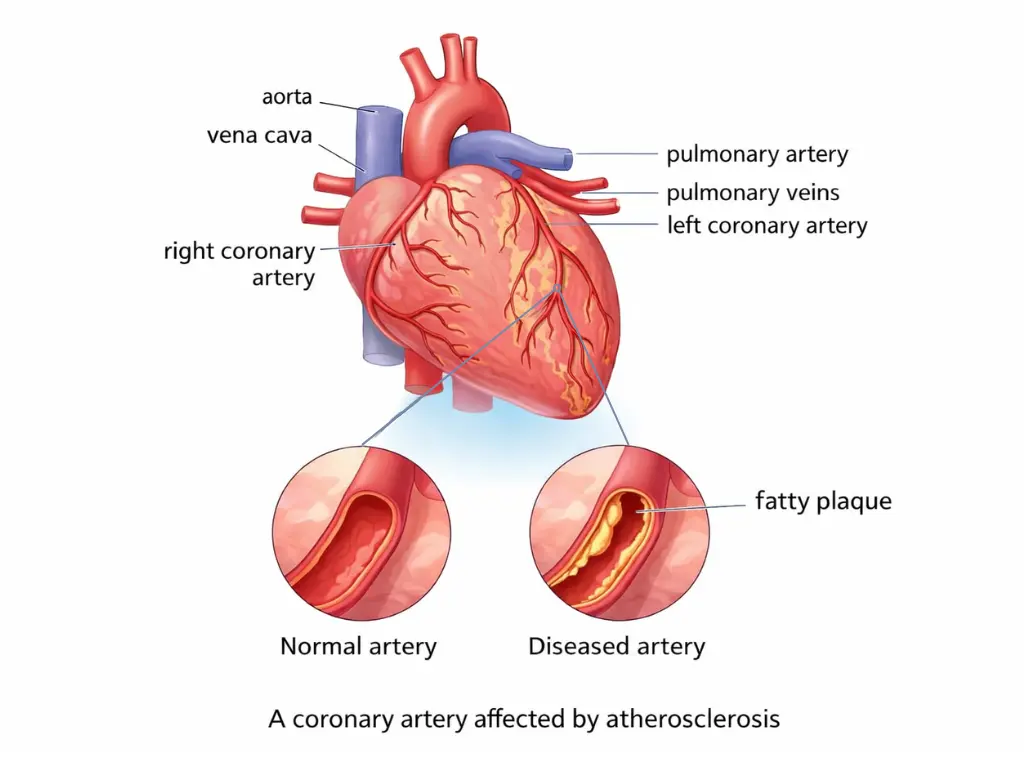
Coronary heart disease (CHD) happens when the blood vessels that feed your heart muscle (your coronary arteries) get narrowed over time by a buildup called plaque.
Think of plaque like a sticky mix of “gunk” (cholesterol and other material) that lines the inside of the artery. Over time, that lining can:
- Narrow the space blood can flow through
- Make the artery less flexible
- Sometimes crack open and trigger a clot (which can block blood flow suddenly)
When your heart muscle can’t get enough oxygen-rich blood, you may develop symptoms—especially with activity, stress, or illness.
CHD often develops quietly. Many people don’t feel anything until the heart starts “asking for more oxygen than the narrowed vessel can deliver.”
Is coronary heart disease the same as coronary artery disease?
This confuses a lot of people, and honestly, it’s understandable.
In everyday healthcare language:
- Coronary artery disease (CAD) and coronary heart disease (CHD) are often used interchangeably.
- You’ll also hear ischemic heart disease used as a related term.
So if you’re searching:
- “is coronary heart disease the same as coronary artery disease”
- “is coronary artery disease and coronary heart disease the same”
…you’re not wrong to ask. Most of the time, people are talking about the same underlying problem: plaque narrowing the coronary arteries.
What symptoms can coronary heart disease cause?
Here’s how CHD shows up in real life—without drama, but without minimizing it either.
Common symptom patterns
CHD can cause symptoms like:
- Chest pressure, tightness, heaviness, or squeezing
- Many people don’t describe it as “sharp pain”
- Some call it “a brick on my chest” or “a tight band”
- Shortness of breath
- Sometimes it’s the main symptom (especially during activity)
- Fatigue that feels out of proportion
- “I’m wiped out doing things that used to be easy”
- Nausea, sweaty/clammy feeling, lightheadedness
- Discomfort that travels
- It can move into the jaw, neck, shoulder, back, or arm
Two quick anonymous scenarios (the kind we see)
- Scenario A: A middle-aged guy who says, “Doc, I don’t have pain… it’s more like pressure when I walk fast, and I have to stop to catch my breath.” That pattern matters.
- Scenario B: A busy mom who keeps brushing off “indigestion,” but notices it comes on with activity and eases when she rests. That’s worth taking seriously.
Why symptoms vary so much
Your heart is not the same as your neighbor’s heart. Symptoms can vary because of:
- Age
- Diabetes
- Fitness level
- Other lung or stomach conditions
- Where plaque is located
- How quickly things are changing
If you’re reading this thinking, “Mine doesn’t sound classic,” that doesn’t automatically make it safe.
What causes coronary heart disease (and who is more likely to get it)?
what causes coronary heart disease is another high-intent question—and it’s not just “bad genes” or “bad diet.”
CHD is usually the result of atherosclerosis (plaque buildup). Risk tends to rise when these factors stack up:
Risk factors we commonly talk about
- High blood pressure
- High cholesterol
- Diabetes / insulin resistance
- Smoking or tobacco exposure
- Family history of early heart disease
- Carrying extra weight (especially around the midsection)
- Lack of regular activity
- Poor sleep and untreated sleep apnea
- Long-term stress (not as the only cause, but as a contributor)
Doctor-to-patient truth: Nobody “earns” heart disease. This isn’t about blame. It’s about understanding what’s modifiable and what needs medical support.
How to check for coronary heart disease
People often ask, how to check for coronary heart disease because they want certainty.
Here’s the honest answer: we usually don’t diagnose CHD from one clue. We connect the dots from symptoms, risk factors, and testing.
Step 1: The conversation matters
A clinician will typically ask about:
- What you feel and when it happens
- What makes it better/worse
- Your medical history and family history
- Smoking history and activity level
Step 2: Common tests that help clarify the picture
Depending on the situation, testing might include:
- An EKG/ECG
- Helpful for rhythm issues or signs of reduced blood flow
- Not a perfect “yes/no” test for CHD by itself
- Blood tests
- Can check for heart strain or heart muscle injury
- Also helps assess risk factors (cholesterol, blood sugar, etc.)
- Imaging-based evaluation
- Sometimes a stress test
- Sometimes a CT-based look at coronary arteries
- In certain cases, cardiac catheterization (a direct look at the arteries)
Practical takeaway: If symptoms are concerning, we don’t rely on “wait and see.” We evaluate.
Treatment and prevention: what actually helps
Let’s cover two common searches here:
- how can we prevent coronary heart disease
- how to reverse coronary heart disease
Prevention (and “getting ahead of it”)
Prevention is not perfection. It’s consistent basics done well:
- Quit tobacco (if applicable) — it’s one of the biggest levers
- Move most days (even walking is meaningful)
- Eat in a way your body can sustain
- More whole foods
- Less ultra-processed
- Less sugary drinks
- Manage blood pressure, cholesterol, and diabetes
- Often requires meds, and that’s not failure—that’s treatment
- Protect sleep
- Follow up consistently (this matters more than a “perfect month”)
“Can coronary heart disease be reversed?”
You’ll see people search:
- can coronary heart disease be reversed
- can you reverse coronary heart disease
- how to reverse coronary heart disease
Here’s the calm, honest version:
- In many people, we can slow progression, stabilize plaque, and lower the risk of heart attack dramatically.
- In some cases, with aggressive risk-factor control, plaque burden may improve over time—but it’s not a guarantee, and it’s not something you “DIY” with supplements.
If you want to think of it simply:
- The goal is safer arteries, better blood flow, and lower risk, not chasing a miracle phrase like “fully reversed.”
What treatment may include
Treatment depends on severity and symptoms, but usually involves:
- Lifestyle changes (the foundation)
- Medications that:
- Lower cholesterol
- Control blood pressure
- Reduce clot risk in appropriate patients
- Improve symptoms like angina
- Procedures when needed:
- Stents (angioplasty)
- Bypass surgery in certain patterns of disease
Warning symptoms that shouldn’t wait
If you take only one section seriously, take this one.
Get urgent evaluation for symptoms like:
- New or worsening chest pressure, tightness, heaviness, or pain
- Chest discomfort plus shortness of breath
- Chest symptoms plus sweating, nausea, or feeling faint
- Trouble breathing at rest or breathing that suddenly worsens
- Fainting or near-fainting with chest symptoms
- Symptoms that feel like “something is wrong” and are not normal for you
You don’t need to prove it’s your heart before you seek help. That’s our job.
If you’re experiencing concerning chest discomfort, unexplained shortness of breath, or any warning symptoms that shouldn’t wait—and you’re in or near Angleton or Brazoria County—it’s reasonable to get evaluated promptly.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.
Frequently Asked Questions
What is coronary heart disease?
Coronary heart disease is plaque buildup in the arteries that supply blood to your heart muscle, which can reduce blood flow and lead to symptoms like chest pressure or shortness of breath.
What is the definition of coronary heart disease?
It’s a condition where the coronary arteries can’t deliver enough oxygen-rich blood to the heart muscle because plaque narrows the artery.
What is a coronary heart disease?
People sometimes search this exact phrase, but it’s referring to the same condition: coronary heart disease, meaning narrowing of the heart’s arteries from plaque.
Is coronary heart disease the same as coronary artery disease?
Most of the time, yes—people use the terms interchangeably. Both refer to plaque narrowing the coronary arteries.
How to check for coronary heart disease?
Evaluation usually includes symptom review, risk-factor assessment, and testing such as an EKG, blood work, and sometimes stress testing or imaging-based assessment.
Can coronary heart disease be reversed?
In many people, we can slow progression and stabilize plaque while reducing risk significantly. True “reversal” isn’t guaranteed, but outcomes can improve a lot with the right plan.