If you searched “what are the 4 stages of congestive heart failure,” you’re probably trying to do something very human:
You’re trying to understand what’s happening—without spiraling.
Let’s slow it down and make it practical.
When doctors talk about “stages,” we’re usually referring to a 4-stage system (A–D) that helps describe risk, heart changes, and symptoms over time. It’s not meant to scare you. It’s meant to guide decisions—what to monitor, what to treat, and how urgently to act if symptoms change.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.
A quick anonymous scenario
Someone comes in from Angleton/Brazoria County and says:
- “I’m not collapsing… but I’m more winded than I used to be.”
- “My ankles are swelling by evening.”
- “I’m sleeping propped up.”
- “I keep telling myself it’s stress or getting older—but it’s getting worse.”
They’re not looking for a label. They’re looking for clarity:
Is this something I can watch… or something I shouldn’t ignore?
That’s exactly what staging is supposed to help with.
what “CHF” and “heart failure” actually mean
Heart failure doesn’t mean your heart “stopped.” It means your heart isn’t pumping or filling as effectively as your body needs.
“Congestive” is commonly used when fluid backup (congestion) is part of the picture—like fluid in the lungs or swelling in the legs.
Think of heart failure less as a single disease, and more as a condition where your heart can’t keep up with your body’s demands. This can happen if the heart muscle is weakened, damaged, or just not functioning as efficiently as it should—sometimes from a heart attack, high blood pressure, valve problems, or other causes.
Because the heart can’t pump blood the way it should, fluid may build up in places it shouldn’t—like your lungs (leading to shortness of breath), your liver, or your ankles. You might hear doctors talk about “left-sided” or “right-sided” heart failure:
- Left-sided heart failure tends to cause fluid to back up into the lungs, making it harder to breathe.
- Right-sided heart failure usually leads to swelling in the legs, feet, or abdomen.
Understanding exactly how and where the heart is struggling helps your healthcare team decide on the best approach for you.
How symptoms differ: Left-sided vs. right-sided heart failure
You might hear doctors mention the “left” or “right” side of the heart when discussing heart failure—and yes, that direction actually matters for symptoms.
- Left-sided heart failure tends to send fluid backward into the lungs. The result? Shortness of breath (especially when lying flat), coughing, and that feeling of being winded after mild activity or even at rest. People may also notice trouble breathing at night or waking up gasping.
- Right-sided heart failure, on the other hand, is more likely to cause fluid to build up in the rest of the body. That can mean swelling in the ankles, feet, or abdomen, and sometimes feeling unusually bloated or noticing rings getting tighter on your fingers by evening.
Bottom line:
Left-sided = more lung and breathing issues.
Right-sided = more swelling and fluid in legs, belly, or hands.
Of course, plenty of people have some of both (called “congestive” for a reason), but recognizing where symptoms show up can clarify what’s happening.
Left vs Right Sided Heart Failure: Where the Problem Starts (and the Clues It Leaves)
The heart’s two sides have their own jobs—and when either side struggles, the symptoms often tell you where things are going awry.
- Left-sided heart failure is the usual suspect. Here, the heart can’t efficiently push blood out to your body, so pressure backs up into the lungs. That’s why you might notice shortness of breath, wheezing, or a cough (especially at night or when lying flat).
- Right-sided heart failure tends to show up as swelling. When the right side isn’t pumping well, fluid backs up in places like the ankles, legs, or even the belly—think “puffy socks by evening” or suddenly tighter waistbands.
It’s possible to have both sides involved over time. Knowing which symptoms show up first helps doctors zero in on what your heart needs most.
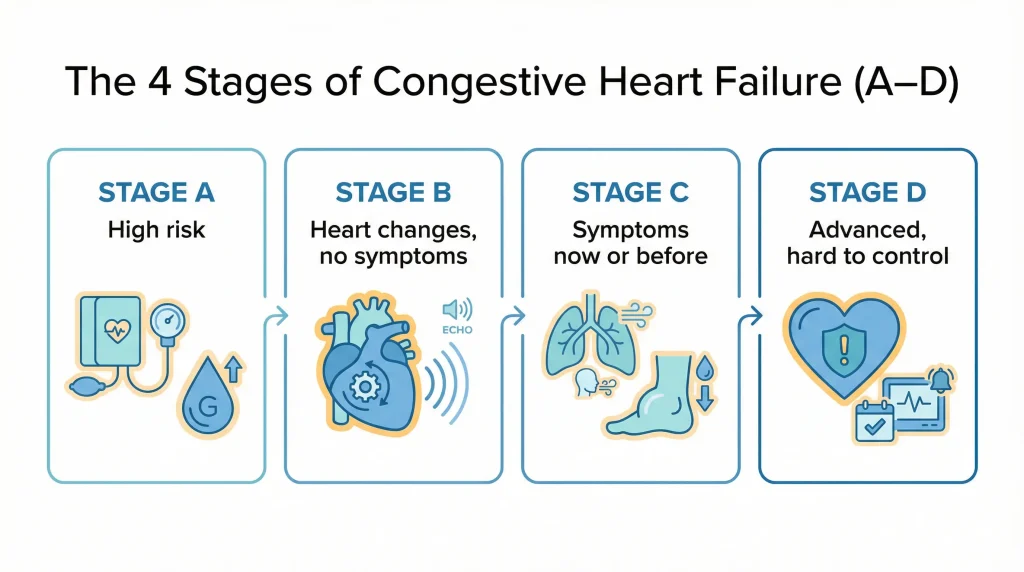
The 4 stages of congestive heart failure (the A–D system)
People often call these “Stage 1–4,” but in most medical settings you’ll hear them as Stage A, B, C, and D.
Stage A: High risk — but no heart damage and no symptoms
This stage means:
- You may have risk factors (like high blood pressure, diabetes, coronary artery disease, obesity, smoking history, or a strong family history)
- No known structural heart changes
- No heart failure symptoms
What it can feel like:
Often… it feels like nothing. And that’s the point—this is where prevention matters most.
What typically helps at this stage (big picture):
- Treating risk factors consistently
- Lifestyle changes that are sustainable (not extreme)
Stage B: Heart changes are present — but no heart failure symptoms yet
This stage means:
- There’s evidence of heart structure/function changes (your clinician might see this on imaging like an echocardiogram)
- But you don’t have heart failure symptoms
What it can feel like:
Still may feel normal day-to-day.
Why this stage matters:
This is often the window where good medical follow-up can delay or prevent symptoms later.
Stage C: Heart changes + symptoms (now or in the past)
Stage C means:
- Heart changes are present and
- You have current symptoms or you’ve had symptoms before
This is where many people first realize: “Okay—this is real.”
What it can feel like (real-life language):
- Getting winded doing normal activities
- Needing more breaks than usual
- Swelling in ankles/legs
- A cough or “chest congestion” that doesn’t behave like a typical cold
- Sleeping propped up because lying flat feels worse
- A noticeable drop in stamina that feels out of proportion
Stage C includes current OR previous symptoms—so even if you’re feeling better today, your medical team may still refer to Stage C if you’ve had symptom episodes before.
Stage D: Advanced heart failure — symptoms are difficult to control
Stage D means:
- Heart failure is advanced and
- Symptoms can be severe, frequent, or hard to manage despite treatment
- People may need specialized therapies and close follow-up
What it can feel like:
- Shortness of breath with minimal activity—or sometimes even at rest
- Frequent flare-ups of swelling/fluid overload
- Very limited stamina
- More urgent visits or hospitalizations
This is the stage that makes people ask the hardest questions. If that’s you, we want you to hear this clearly:
Stage D is not a verdict. It’s a way to signal that your care may need to be more specialized and more tightly managed.
How quickly can heart failure progress—and what makes the difference?
There’s no single timetable for how heart failure unfolds. For some, symptoms barely budge for years, held steady with good follow-up and a little luck. For others, things can change more quickly—sometimes over months, or even weeks.
A few big factors shape the pace:
- Underlying cause: Heart failure due to long-standing high blood pressure or valve disease may smolder for ages. But a heart weakened suddenly (like after a heart attack or a virus) often has a steeper climb.
- How well risk factors are managed: Blood pressure, blood sugar, cholesterol, and sticking with medications make a massive difference.
- Lifestyle choices: Smoking, ongoing alcohol use, skipping out on follow-ups, or ignoring salt/fluid guidance can tip the balance toward faster progression.
- Any new strains on the heart: Infections, uncontrolled arrhythmias (like atrial fibrillation), or new blockages can move the needle from stable to shaky.
What’s most important: regular check-ins. Even when it feels like “just a little more tired,” a pattern of change is worth catching early. Heart failure can be slow, steady, or sometimes throw a curveball—and the sooner you spot a shift, the more options you—and your clinical team—have.
“Stages” vs “Classes”
You’ll also see “Classes I–IV” online. That’s usually the NYHA functional classification, which is a different system.
Here’s the simplest way to think about it:
- Stages (A–D) describe risk and heart disease progression
- Classes (I–IV) describe how limited you feel by symptoms right now
Quick cheat sheet (NYHA classes):
- Class I: No symptoms with normal activity
- Class II: Symptoms with more-than-usual exertion (some limitation)
- Class III: Symptoms with minimal activity (marked limitation)
- Class IV: Symptoms even at rest
A person can be Stage C (because they’ve had symptoms) but be Class II on a good month and Class III during a flare. That’s one reason you’ll see different “labels” at different times.
How doctors actually use staging
When staging is used well, it helps guide:
- How closely you should be followed
- What kinds of medications or therapies might be considered
- Whether we’re focusing on risk reduction, symptom control, or advanced management
- How seriously we take symptom changes (especially breathing changes)
What staging should not do:
- It should not be used as a “countdown clock.”
- It should not replace an actual evaluation when symptoms change.
Can you move “backwards” to an earlier stage of heart failure?
This is a common question—and a really natural one. Here’s the practical answer:
Once the heart has developed structural changes (think Stage B or later), those changes usually don’t fully “reverse,” even with the best care. So, in terms of A–D staging, the clock doesn’t technically roll backward.
But there’s good news: how you feel (your NYHA class) can absolutely improve with the right treatment plan. Better symptom control, more energy, and the ability to do more daily activities is possible—even if your official stage doesn’t change.
Bottom line: while the underlying heart structure may not rewind, many people do move to feeling better and living more fully thanks to advances in medications, lifestyle changes, and regular follow-up. That’s something worth focusing on.
Diagnosis: how heart failure is evaluated
If a clinician suspects heart failure, diagnosis usually includes a mix of:
- History + exam (symptom pattern and changes over time)
- Blood tests (can help detect heart strain and check how other organs are handling fluid balance)
- EKG (checks electrical rhythm and signs of strain/previous injury patterns)
- Chest imaging (can help assess congestion/fluid patterns and other causes of shortness of breath)
- Echocardiogram (ultrasound of the heart) (helps evaluate structure and function)
Sometimes additional testing is needed depending on the situation and the suspected cause.
Treatment: what typically happens by stage
Treatment is individualized, but the big framework often looks like this:
Stage A (risk reduction)
- Control blood pressure, diabetes, cholesterol (when applicable)
- Stop smoking (if relevant)
- Heart-healthy activity and nutrition that you can sustain
- Address sleep issues, alcohol use, weight, and stress patterns (as appropriate)
Day-to-day strategies for living well at any stage:
- Take medications exactly as prescribed (if any are recommended)
- Stick to a heart-healthy diet, focusing on lower sodium and saturated fats
- Monitor your weight—let your care team know if you notice sudden changes
- Stay physically active as advised by your doctor (even gentle movement counts)
- Manage stress with relaxation techniques or counseling if it helps
- Limit alcohol consumption
- Don’t skip medical appointments—regular check-ins matter
- Learn about your condition and keep asking questions
- Lean on support from family, friends, or support groups when you need it
Stage B (treat heart changes early)
- Ongoing risk reduction
- Medications may be started to reduce strain and prevent progression (your clinician decides what fits)
At this stage, you might start to notice that everyday activities feel a bit harder—maybe you get unusually tired or a little short of breath doing things that didn’t bother you before. This is often the point where healthcare providers get more proactive, recommending aggressive management to slow or prevent things from getting worse. Along with lifestyle modifications, your clinician may prescribe medications like ACE inhibitors or beta-blockers to help protect your heart’s function and reduce the risk of moving into a symptomatic stage. The overall goal here is to catch changes early and keep symptoms at bay for as long as possible.
Stage C (treat symptoms + the underlying cause)
- Medication plans often expand here to control symptoms and reduce flare-ups
- Managing triggers (dietary sodium sensitivity, missed meds, kidney strain, infections, rhythm problems, etc.) becomes a big part of stability
- Follow-up becomes more structured
At this stage, treatment generally becomes more intensive and multi-faceted. Multiple medications are usually involved—for example, diuretics may be added to remove extra fluid, while other meds are targeted to support heart function and ease symptoms. Lifestyle changes (especially regarding diet, daily activity, and monitoring fluid intake) take on even more importance, and it’s common to need closer medical monitoring.
Regular follow-up visits and periodic testing are key at this point. These check-ins help your care team track how you’re doing, monitor for any progression, and adjust your treatment plan as needed to keep symptoms in check and prevent hospitalizations.
Stage D (advanced management)
- Closer monitoring
- Specialized therapies (depending on the person’s situation)
- A stronger emphasis on quality of life and preventing repeated severe flare-ups
At this point, heart failure is considered advanced or end-stage. Symptoms are often severe and can show up even at rest, making daily activities—sometimes even walking a block—very challenging. People in Stage D typically experience:
- Persistent symptoms that don’t improve with standard medicines
- Frequent or repeated hospitalizations and emergency room visits
- Marked limitations in physical activity and energy
- Significant impact on daily life, with other organs often feeling the effects
Because treatment options may be more limited, conversations here usually focus on comfort, stability, and what matters most to you. Depending on the situation, your care team might discuss options like heart pumps (mechanical assist devices), transplant (for select candidates), continuous IV medications, or support through palliative or hospice care. The goal is to tailor care to your needs, prioritize quality of life, and help avoid repeated, severe flare-ups.
Medications commonly used in heart failure
A wide range of medications play a role in heart failure treatment, and your exact combination can depend on your stage, symptoms, and any other medical conditions. Some of the main types include:
- ACE inhibitors and ARBs: These help relax blood vessels and reduce strain on the heart.
- Beta-blockers: Slow the heart rate and can help prevent further damage.
- Diuretics: Sometimes called “water pills,” these help the body get rid of excess fluid, easing swelling and shortness of breath.
- Aldosterone antagonists: Target hormones that can contribute to fluid retention and heart remodeling over time.
- SGLT2 inhibitors: A newer group originally for diabetes, but found helpful for many people with heart failure—even without diabetes.
Your clinician will tailor your regimen based on your unique situation, sometimes adjusting medications as your symptoms and stage shift. Titling (careful adjustment of dose) and monitoring for side effects are both important parts of the process.
Is Exercise Safe for People With Heart Failure?
Great question. In many cases, exercise can be a positive, even essential, part of heart failure management—but it does need to be customized. The type and intensity of activity should be tailored to your unique situation, and your care team will play a crucial role in helping you determine what’s both safe and beneficial.
A few key points to remember:
- Exercise often helps improve stamina, strength, and even symptoms over time.
- Not all activities are a good match. What’s right for one person may be too much for someone else, depending on stage and symptoms.
- Your doctor or cardiologist can help guide you toward a supervised or structured program if needed—often called cardiac rehab.
Precautions to keep in mind:
- Always check with your clinician before starting or changing an exercise routine.
- Pay attention to your body: if you notice new or worsening symptoms (chest pain, unusual shortness of breath, palpitations, dizziness), stop and let your provider know.
- Some days will be better than others. It’s okay (and expected) to adjust your activity depending on how you feel.
Bottom line: For many people living with heart failure, movement is part of feeling better—but your safety comes first. It should always be a collaborative effort with your care team.
If you’re reading this and thinking, “I don’t know what stage I’m in,” that’s normal. It’s a reasonable question to ask your clinician directly.
Can heart failure be cured or reversed?
This is a common—and important—question. The short answer: for most people, heart failure isn’t something that can be fully “cured” in the sense of making it disappear entirely. That said, “reversal” is a bit more nuanced.
If someone is in the earlier stages (particularly before structural heart changes have set in), aggressive management of risk factors—think high blood pressure, diabetes, cholesterol, or sleep apnea—can absolutely slow or even halt progression. In a few scenarios (like if heart function drops from a brief, reversible insult, such as certain infections or severe rhythm problems), people can sometimes recover normal function. But once lasting structural changes to the heart have happened (Stages B, C, or D), those changes are generally not reversible.
Here’s the encouraging part: even if we can’t turn back time on heart muscle structure, there’s a lot that can be done to improve how you feel and function day to day. With guideline-directed medications, targeted therapies, and solid self-care, many people move from barely making it up the stairs to resuming parts of their old routines. In fact, folks often “move up” the NYHA class scale—meaning less limitation and better symptom control—despite living with an underlying diagnosis.
In other words: we may not cure the condition, but with the right plan, life can get a lot better.
Warning symptoms that shouldn’t wait
If you or a loved one might have heart failure—or you’ve already been told you do—these are warning symptoms that shouldn’t wait:
- Severe or rapidly worsening shortness of breath (especially at rest)
- New or worsening chest pain, pressure, or tightness
- Fainting, near-fainting, severe weakness, or new confusion
- Bluish lips/face or obvious breathing distress
- A very fast or irregular heartbeat with feeling unwell
- Symptoms clearly escalating compared to your usual baseline
If you’re on the fence, it’s reasonable to get evaluated. With breathing and chest symptoms, guessing wrong can get dangerous.
If you’re experiencing new or worsening shortness of breath, swelling, chest discomfort, or a symptom pattern that feels “off”—and you’re in or near Angleton or elsewhere in Brazoria County—it’s reasonable to get evaluated.
At Angleton ER, we’re open 24/7, with board-certified physicians and on-site diagnostics (including imaging and lab testing) to help sort out whether symptoms are heart-related, lung-related, or something else that needs attention.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.
Frequently Asked Questions
What are the 4 stages of congestive heart failure?
Most clinicians refer to Stage A, B, C, and D. Stage A is risk only, Stage B is heart changes without symptoms, Stage C includes current or prior symptoms, and Stage D is advanced heart failure that can be difficult to control.
What is Stage 4 heart failure?
People often say “Stage 4” when they mean Stage D (advanced heart failure) or sometimes NYHA Class IV (symptoms at rest). These are different systems—so it’s worth asking your clinician which one they’re using.
What is Stage C heart failure?
Stage C means there are heart changes and you have symptoms now or you’ve had symptoms in the past. Even if you feel okay today, a prior symptom episode can keep you in Stage C.
What is end-stage heart failure?
“End-stage” is often used informally to describe advanced heart failure (Stage D). It does not automatically tell you “how long” someone has. It signals that symptoms may be hard to control and care may need to be more specialized and more closely managed.
How many stages of heart failure are there?
In the commonly used staging system, there are four stages (A–D). You may also see four NYHA classes (I–IV), which describe symptom limitation rather than disease progression.