Hearing “stage 4 chronic kidney disease” can feel overwhelming. For many people, this is the point where kidney disease starts sounding much more serious, and naturally, the questions become more urgent: What does stage 4 actually mean? What symptoms should I expect? What am I supposed to eat now? The good news is that stage 4 CKD is serious, but it is also the stage where clear information, careful follow-up, and the right plan can still make a real difference.
Medical disclaimer: This article is for educational purposes only. It is not medical advice, diagnosis, or a substitute for care from a licensed healthcare professional. Diet changes, medicines, and follow-up plans for stage 4 CKD should be individualized.
What stage 4 chronic kidney disease means
Chronic kidney disease means the kidneys have been damaged over time and are not doing their jobs as well as they should. Those jobs include removing waste and extra fluid, helping control blood pressure, balancing minerals, and supporting red blood cell and bone health.
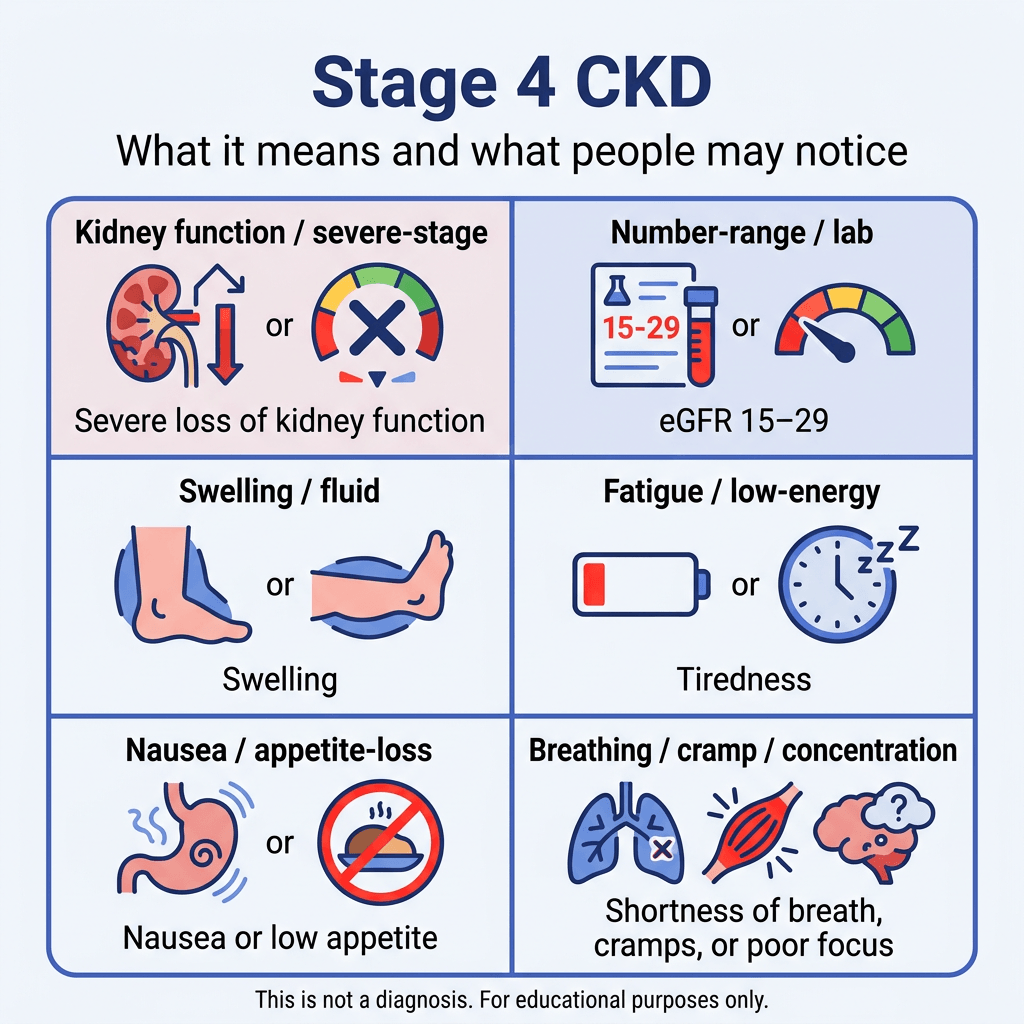
Stage 4 CKD means severe loss of kidney function. In practical terms, it usually means an eGFR of 15 to 29 for 3 months or more. Another way to understand it is that the kidneys are working at a much lower level than normal, but this is still not the same as stage 5 kidney failure.
Stage 4 is different from stage 3 because symptoms are often more noticeable, complications become more common, and the risk of progressing to kidney failure becomes much higher. This is also the stage where planning ahead matters more, including seeing a kidney specialist regularly and getting clearer about treatment and nutrition decisions.
What happens in the body during stage 4 CKD
At this stage, the kidneys have a harder time handling waste, fluid, and mineral balance. That can affect many parts of the body at once. Waste products may build up more easily, extra fluid may be harder to remove, and imbalances in potassium, phosphorus, calcium, and acid levels can become more important.
Stage 4 CKD is also tied to a higher risk of heart disease and high blood pressure, even apart from the kidney problem itself. National Kidney Foundation guidance notes that people with stage 4 CKD are at the highest risk for kidney failure and at very high risk for heart disease.
That is why stage 4 is not just about “kidney numbers.” It is about how the kidneys, heart, blood, bones, fluids, and blood vessels all start affecting one another more strongly.
Common symptoms of stage 4 chronic kidney disease
Symptoms are common in stage 4 CKD, although not every person feels them the same way. National Kidney Foundation lists symptoms such as urinating more or less often than usual, itchy or dry skin, feeling tired, trouble concentrating, numbness or swelling in the arms, legs, ankles, or feet, muscle cramping, shortness of breath, nausea, vomiting, loss of appetite, trouble sleeping, and breath that smells ammonia-like.
A lot of these symptoms happen because the kidneys are no longer keeping the body in balance as smoothly as before. Fluid can build up, appetite can drop, waste products can affect how you feel, and complications like anemia can add to fatigue and weakness.
One important point: symptoms can vary. Some people notice swelling and tiredness first. Others notice nausea, itching, sleep problems, or a drop in appetite. Some feel worse very gradually, while others notice a sharper change after lab work already showed the kidneys were struggling.
Complications that often become more important in stage 4
Stage 4 CKD is also when several complications often start showing up more clearly. National Kidney Foundation specifically lists:
- anemia
- metabolic acidosis
- mineral and bone disorder
- hyperkalemia (high potassium)
Anemia matters because it can worsen tiredness, weakness, and shortness of breath. NIDDK explains that anemia is common in CKD and often becomes more likely as kidney disease gets worse.
Metabolic acidosis means too much acid can build up in the blood. Mineral and bone disorder means calcium and phosphorus balance is being disrupted in ways that can affect bones and blood vessels. Hyperkalemia matters because high potassium can affect the heart and muscles. These are exactly the kinds of issues that make regular lab monitoring much more important in stage 4.
Why diet questions become more important in stage 4 CKD
By stage 4, diet advice becomes much more important because what you eat and drink can affect symptoms, lab values, fluid balance, and how well treatment works. NIDDK explains that choosing healthy foods and avoiding foods high in sodium, potassium, and phosphorus may help prevent or delay some CKD-related problems, and that nutrition needs change as CKD advances.
This is also why stage 4 diet advice is not the same for every patient. Two people can both have stage 4 CKD and still need different nutrition changes depending on blood pressure, diabetes, potassium level, phosphorus level, appetite, weight, and whether swelling or fluid retention is part of the problem.
So when people ask for a “stage 4 CKD diet,” the most honest answer is that there are common themes, but there is no one meal plan that safely fits everybody.
Common diet questions people ask in stage 4 CKD
Do I need to lower sodium?
Very often, yes. NKF says stage 4 CKD usually requires limiting sodium, and NIDDK explains that too much sodium causes the body to hold on to fluid, which can worsen swelling and raise blood pressure. A common upper limit for adults is 2,300 mg per day, though some people need a lower target.
Do I need to watch potassium?
Maybe, and the answer depends a lot on your blood tests. NIDDK explains that CKD can make it harder for the kidneys to remove potassium from the blood, and potassium can become dangerously high in some people. But not everyone with stage 4 CKD has the exact same potassium restriction.
Do I need to limit phosphorus?
Often this becomes a more common issue at stage 4. Damaged kidneys do not remove phosphorus as well as healthy kidneys do, so phosphorus can build up in the blood. NIDDK notes that too much phosphorus can harm blood vessels and weaken bones, which is why processed foods with phosphorus additives often need more caution.
What about protein?
Protein is still important, but more is not always better. NIDDK explains that some people with CKD may need moderate amounts of protein so waste does not build up too much in the blood, while too little protein can lead to malnutrition. In other words, protein in stage 4 CKD usually needs balance, not extremes.
Do I need to change calcium or fluid intake?
Possibly. Calcium concerns often connect to mineral and bone disorder, and fluid intake may need adjustment depending on swelling, urine output, and overall kidney function. NIDDK specifically says some people with CKD may need to adjust how much liquid they consume each day.

Foods and habits that often need more caution in stage 4 CKD
At this stage, people often need to be more careful with:
- high-sodium packaged foods, including canned soups, frozen meals, processed meats, chips, crackers, and salty sauces
- processed foods with phosphorus additives
- potassium-heavy foods if potassium is running high
- salt substitutes with potassium chloride
- over-the-counter supplements or herbal products that have not been reviewed by a clinician or pharmacist
Label reading becomes much more important here. NIDDK recommends checking the Nutrition Facts label for sodium and the ingredient list for phosphorus additives, including ingredients with “PHOS” in the name.
Questions to ask about your stage 4 CKD diet
A very practical next step is to stop trying to guess everything alone and ask more targeted questions, such as:
- Which nutrients do I need to watch most right now?
- Are my current labs showing a potassium or phosphorus problem?
- Do I need a kidney dietitian?
- Are my vitamins, powders, or supplements safe for stage 4 CKD?
- How often should my labs be checked?
These questions matter because stage 4 CKD nutrition is much safer when it is based on actual lab results and symptoms rather than generic internet lists.
Other steps that matter in stage 4 CKD
Diet is important, but it is not the whole plan. Stage 4 CKD management also depends on:
- blood pressure control
- diabetes control, if diabetes is present
- reviewing medicines carefully
- avoiding NSAIDs unless a clinician says otherwise
- regular nephrology follow-up
- planning ahead for future treatment discussions if kidney function keeps falling
NKF specifically warns that by stage 4, some medicines may start building up in the body and some may become unsafe. It also specifically says NSAIDs should generally be avoided in stage 4 CKD.
When stage 4 CKD symptoms should not wait
Some symptoms deserve faster medical attention instead of routine follow-up. These include:
- shortness of breath
- severe swelling
- repeated vomiting
- confusion
- very little urine
- rapidly worsening weakness
Those symptoms can signal more serious fluid overload, worsening waste buildup, metabolic imbalance, or another urgent problem. They should not be brushed aside as “just part of kidney disease.”
For people in Angleton and Brazoria County, one of the hardest parts of stage 4 CKD is knowing when symptoms are part of a chronic condition and when they have crossed into something more urgent. If breathing feels harder, vomiting keeps happening, swelling is getting more severe, or weakness and confusion are worsening, Angleton ER can evaluate urgent symptoms and help guide what follow-up needs to happen next.
Frequently Asked Questions
What does stage 4 CKD mean exactly?
It means severe loss of kidney function, usually with an eGFR of 15 to 29 for 3 months or more.
Is stage 4 CKD considered kidney failure?
No. Stage 4 is severe CKD, but stage 5 is the stage called kidney failure.
What symptoms are common in stage 4 CKD?
Common symptoms include swelling, tiredness, itching, trouble concentrating, nausea, vomiting, appetite loss, shortness of breath, muscle cramping, and urine changes.
Do all people with stage 4 CKD need a special diet?
Most need some nutrition changes, but not all need the exact same restrictions. Stage 4 diet advice is individualized.
Do I need to avoid potassium in stage 4 CKD?
Not automatically. Potassium changes depend on your lab results and clinical situation.
Is phosphorus a problem in stage 4 CKD?
It often becomes more important because damaged kidneys do not remove phosphorus as well, and high phosphorus can harm bones and blood vessels.
How much protein should someone with stage 4 CKD eat?
There is no single amount that fits everyone. Many people need a more moderate protein intake, but the right amount should be individualized.
Can stage 4 CKD get better?
It is usually treated as a chronic condition that may worsen over time, but treatment can help slow progression and lower complications.
When should someone see a kidney specialist?
At stage 4, nephrology follow-up is especially important because complications, medicine safety, and future planning all matter more.
When should stage 4 CKD symptoms be treated urgently?
When symptoms include severe shortness of breath, major swelling, repeated vomiting, confusion, very low urine output, or rapid decline.