If you have stage 4 chronic kidney disease, protein becomes one of the most confusing parts of the diet. Many people hear they need to “cut back,” but then worry about getting weak or not eating enough. The most accurate answer is this: in stage 4 CKD not on dialysis, many people are advised to eat less protein than average, but not too little. The goal is usually to lower the amount of protein waste the kidneys have to handle while still protecting muscle, strength, healing, and overall nutrition.
For people in Angleton and across Brazoria County, the protein question usually becomes urgent when stage 4 CKD is diagnosed and appetite, labs, or weight are already starting to change. The safest way to think about protein at this stage is not “high protein” or “no protein.” It is the right amount for your body, your labs, and whether you are on dialysis or not.
Medical disclaimer: This article is for educational purposes only. It is not medical advice, diagnosis, or a substitute for care from a licensed healthcare professional or renal dietitian.
Does stage 4 CKD usually require a lower-protein diet?
In many cases, yes, if you are not on dialysis. NIDDK says some people with CKD may need to consume moderate amounts of protein so waste does not build up in the blood. National Kidney Foundation also says that for people with kidney disease not on dialysis, a lower-protein diet is often recommended because excess protein waste can build up and make the kidneys work harder.
Protein becomes a bigger issue in stage 4 because the kidneys are already working at a much lower level. As your body uses protein, it creates waste products the kidneys must clear. When kidney function is severely reduced, too much protein can increase that burden. NKF says excess protein waste can build up in the blood and may contribute to symptoms such as nausea, loss of appetite, weakness, and taste changes.
At the same time, “lower protein” should never be understood as “almost no protein.” NIDDK warns that too little protein may lead to malnutrition, and NKF says protein needs still depend on body size, nutritional status, and the underlying kidney problem.
How much protein is usually okay in stage 4 CKD?
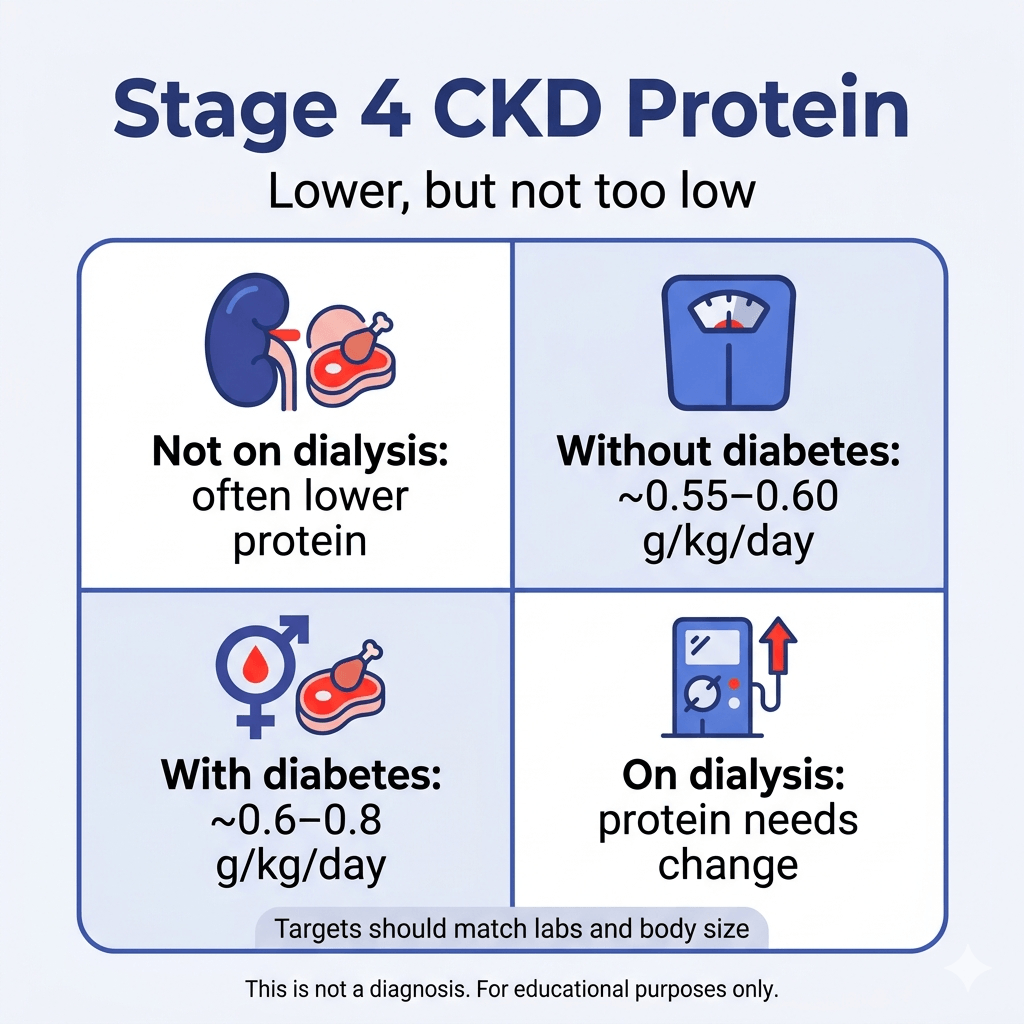
This is where the answer becomes more individualized. A common specialist framework comes from the 2020 KDOQI nutrition guidance. Commentary on that guideline states that for metabolically stable adults with CKD stages 3 to 5 who are not on dialysis and do not have diabetes, protein is often restricted to about 0.55 to 0.60 grams per kilogram of body weight per day. For CKD stages 3 to 5 with diabetes, the recommended range is often a little higher, around 0.6 to 0.8 grams per kilogram per day.
That does not mean everyone should calculate a target and manage it alone. NIDDK and NKF both emphasize that protein needs change over time and should be set with a dietitian or healthcare professional. These numbers are best understood as common clinical guide ranges, not a do-it-yourself prescription.
A simple example can make the range easier to picture. If someone weighs 70 kg (about 154 pounds), then a range of 0.6 to 0.8 g/kg/day would be about 42 to 56 grams of protein per day. A stricter 0.55 to 0.60 g/kg/day approach would be about 38.5 to 42 grams per day. That arithmetic is just an illustration of the guideline ranges above, not a personalized target.
What changes the protein answer in stage 4 CKD?
Two people with stage 4 CKD may get different protein advice. NKF says the right protein amount depends on things like your weight, your age, the amount of protein in your urine, and your type of kidney disease. NIDDK also says protein needs may change over time.
That means the answer may change if you are losing weight, eating poorly, losing significant protein in the urine, also managing diabetes, or starting dialysis soon. A person who is frail or undernourished may need a less aggressive protein reduction than someone who is overweight, stable, and eating well. This is why the stage number alone does not tell the whole story.
Why too much protein can be a problem in stage 4 CKD
Too much protein can make the kidneys work harder because protein metabolism creates waste that has to be cleared from the blood. NKF says this can be stressful for the kidneys and may cause them to wear out faster. It also notes that limiting protein and including more plant-based foods may help slow loss of kidney function in some people who are not on dialysis.
In real life, excess protein can also show up quietly. Large servings of meat, protein-heavy meals at every sitting, and protein powders or shakes can push total intake higher than many people realize. That point is an inference based on the guideline ranges and NKF’s warning that excess protein waste can accumulate and strain the kidneys.
Why too little protein can also be a problem
Protein is still essential. NIDDK says protein helps build and maintain muscle, bone, skin, connective tissue, internal organs, and blood, and it also helps fight disease and heal wounds. If protein intake drops too low, the body can lose muscle and overall nutrition can suffer.
This is especially important in stage 4 CKD when appetite may already be poor. If someone is eating less overall because of nausea, taste changes, or fatigue, cutting protein too aggressively can backfire. NKF and NIDDK both warn that too little protein can lead to weakness and malnutrition.
What kinds of protein are often better in stage 4 CKD?
NIDDK says some people with CKD may be advised to limit meat and dairy foods, get more of the remaining protein from plant-based foods, and choose lean meats that are lower in phosphorus when they do eat animal protein. NKF also notes that plant proteins may be easier on the kidneys and that plant-based eating can help reduce acid load.
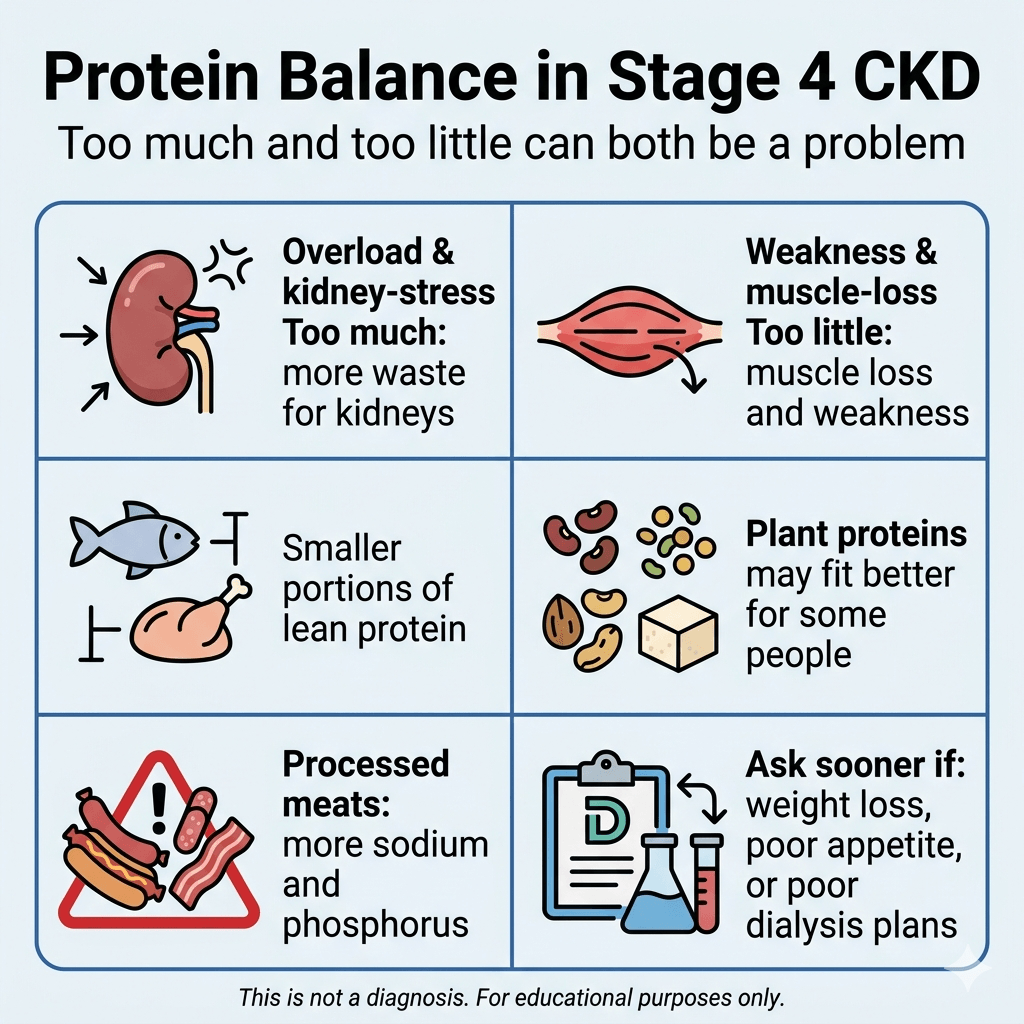
That usually means the protein conversation is not only about how much, but also about what kind. Smaller portions of lean animal protein may fit better than large servings of red meat or processed meat. Plant proteins may also fit well for some people, but they still have to be matched to potassium and phosphorus needs.
Processed meats are usually a poor choice because they tend to bring extra sodium and phosphorus along with the protein. NIDDK and NKF both repeatedly warn that processed foods can create problems not just because of protein, but because of the added sodium and phosphorus load.
How to think about protein across the day
Protein adds up meal by meal, not just at dinner. A moderate portion at breakfast, lunch, and dinner can fit very differently from eating most of the day’s protein in one large meal. This is a practical inference from the body-weight-based intake ranges used in CKD guidance.
It is also worth remembering that supplements and shakes can push protein intake higher very quickly. Someone may think they are eating “lightly” while still going well above their target because of protein bars, powders, drinks, or meal replacements. Again, that is a practical inference from the fact that stage 4 CKD usually requires moderation rather than excess.
What changes if someone with stage 4 CKD is on dialysis?
Dialysis changes the protein answer. NIDDK says people with CKD who are on dialysis may need to eat more protein because dialysis removes protein from the blood. NKF gives the same message: once dialysis starts, a low-protein diet is usually no longer appropriate in the same way.
So if someone has stage 4 CKD and has already started dialysis, they should not follow non-dialysis protein guidance without checking with their dialysis team or renal dietitian. Dialysis creates a different nutrition situation.
Questions to ask about protein in stage 4 CKD
A better conversation with your care team often starts with a few direct questions:
- How much protein should I aim for based on my weight?
- Am I eating too much or too little right now?
- Should I shift more of my protein toward plant sources?
- Are my potassium, phosphorus, or albumin levels changing what is best for me?
- Should I meet with a kidney dietitian?
These questions matter because stage 4 CKD nutrition works best when it is based on actual labs, actual symptoms, and actual intake rather than guesswork.
When protein questions need medical follow-up sooner
Protein intake deserves quicker review if weight loss is happening, appetite is poor, nausea is worsening, labs are changing quickly, or dialysis is starting or being discussed. Those situations can shift the balance between “too much protein” and “not enough protein” very quickly.
It is also worth checking in sooner if protein supplements are being used without guidance. In stage 4 CKD, a supplement that seems harmless can push protein, phosphorus, potassium, or calories in the wrong direction depending on the product and the patient’s labs. That is a practical inference from NIDDK’s and NKF’s repeated guidance to individualize protein and CKD nutrition.
For people in Angleton and Brazoria County, protein questions often come up when stage 4 CKD is already affecting appetite, energy, or lab results. If nausea, vomiting, weakness, weight loss, or other kidney-related symptoms are worsening, Angleton ER can evaluate urgent symptoms and help guide what kind of follow-up needs to happen next.
Frequently Asked Questions
How much protein is okay for stage 4 CKD?
There is no one number for everyone, but common non-dialysis guideline ranges for stage 3 to 5 CKD are around 0.55 to 0.60 g/kg/day without diabetes and around 0.6 to 0.8 g/kg/day when diabetes is present, assuming the person is metabolically stable and not on dialysis.
Should people with stage 4 CKD eat less protein?
Often yes, if they are not on dialysis. NKF says a lower-protein diet is often recommended for kidney disease patients not on dialysis.
Is 0.8 g/kg too much for stage 4 CKD?
Not always. It may still fit some people, especially if diabetes is present or the person is at nutritional risk. The right target depends on the full clinical picture.
What happens if you eat too much protein with stage 4 CKD?
Protein waste can build up in the blood, the kidneys may work harder, and some people may notice nausea, taste changes, weakness, or appetite loss.
Can too little protein be dangerous in stage 4 CKD?
Yes. Too little protein can contribute to malnutrition, weakness, and muscle loss.
Are plant proteins better for stage 4 CKD?
For some people, they may be easier on the kidneys and may reduce acid load, but they still need to fit the person’s potassium and phosphorus needs.
Do protein needs change once dialysis starts?
Yes. People on dialysis usually need more protein because dialysis removes protein from the blood.
Should people with stage 4 CKD use protein shakes?
Not casually. A shake may look helpful but can quietly raise protein intake and sometimes add phosphorus or potassium too. It is better to ask before using them regularly. This is an inference grounded in CKD protein moderation and CKD mineral guidance.
Does diabetes change protein goals in stage 4 CKD?
Yes. KDOQI-based guidance commonly uses a slightly higher protein range in CKD stages 3 to 5 when diabetes is present.
When should someone ask for a kidney dietitian?
As soon as protein targets feel confusing, weight is changing, appetite is poor, labs are worsening, or dialysis is being discussed. NIDDK and NKF both encourage working with a dietitian for CKD nutrition decisions.

