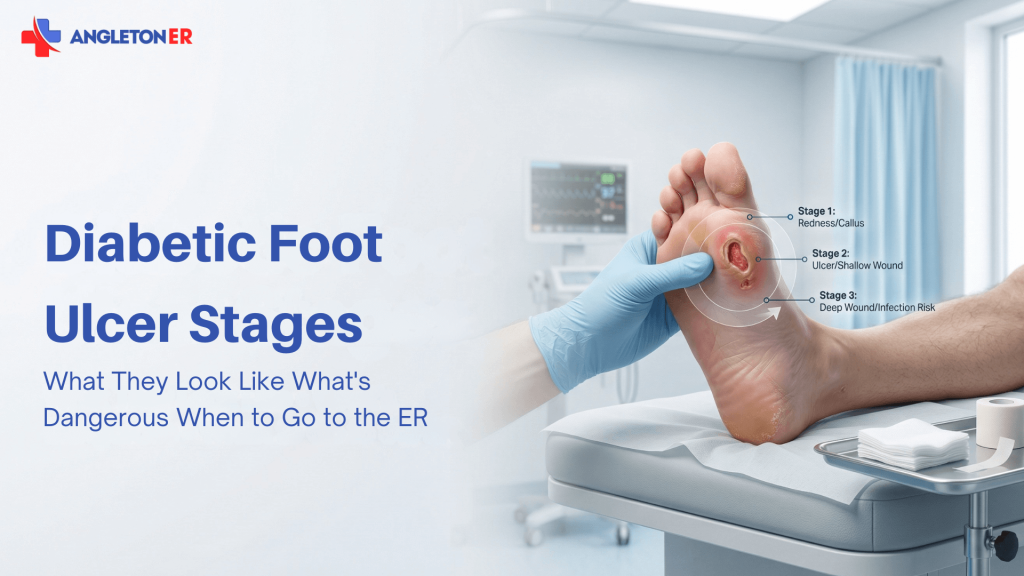
If you’re searching “diabetic foot ulcer stages,” I’m going to assume one thing: you’re worried this is getting worse—and you want to know what “stage” you’re in.
As an ER doctor, I’ll tell you this plainly: staging helps clinicians communicate risk, but you shouldn’t try to stage your own wound at home. What you can do is learn the warning signs that mean infection, tissue death, or bone involvement could be happening—and that’s when time matters.
Here in Angleton, where the 2024 population estimate is 20,979 and 19.1% of residents are 65+, early foot checks matter because neuropathy and circulation problems become more common as we age.
what is a diabetic foot ulcer—and why do “stages” matter?
A diabetic foot ulcer is an open sore/wound on the foot that develops because diabetes can cause:
- nerve damage (you don’t feel injuries), and
- poor blood flow (wounds heal slower and get infected easier).
“Stages” matter because they roughly describe how deep the ulcer goes and whether there are signs of infection or gangrene—and those details change what we do next.
Diabetic foot ulcer stages (Wagner grades 0–5)

Clinicians often use the Wagner (Meggitt-Wagner) grading system as a practical “staging” method. The IWGDF guideline summarizes these grades clearly:
Stage chart
| Wagner Grade | What it usually means (plain English) |
|---|---|
| 0 | High-risk foot / pre-ulcer (callus, deformity, pressure points; skin not broken yet) |
| 1 | Superficial ulcer (skin-level open sore) |
| 2 | Deeper ulcer reaching tendon or joint capsule |
| 3 | Deep ulcer with abscess or bone infection risk (osteomyelitis) |
| 4 | Forefoot gangrene (dead tissue in part of the foot) |
| 5 | Whole-foot gangrene |
What to notice
- Grades 0–1 are the window where we can prevent a spiral.
- Grades 2–3 raise concern for deeper structures and infection.
- Grades 4–5 are emergencies because gangrene can spread and become life-threatening.
What does a diabetic foot ulcer look like?
People ask this a lot: “what does a diabetic foot ulcer look like?” It can vary, but common signs include:
- A red crater or open sore (often on the bottom of the foot or near toes)
- Drainage on socks (clear, yellow, or pus)
- Swelling around the area
- Bad odor
- Black or gray tissue (this can mean dead tissue/gangrene—do not wait)
Important: Some ulcers are hidden under callus. CDC emphasizes daily foot checks because nerve damage can make you miss injuries until they’re serious.
How do diabetic foot ulcers start?
The simplest answer: small injury + you don’t feel it + it doesn’t heal well.
Common starting points:
- A blister from shoes
- A crack in dry skin
- A cut you didn’t notice
- Pressure from a callus
CDC notes nerve damage can cause loss of feeling in the feet and increases risk for ulcers—this is why they recommend checking feet every day.
What causes diabetic foot ulcers to get worse?
If you’re asking “what causes diabetic foot ulcers” to progress, it’s usually one or more of these:
Infection
Foot infections can worsen quickly in diabetes. The IWGDF/IDSA guideline is specifically focused on how serious diabetic foot infections can be and how they should be managed clinically.
Poor circulation (PAD)
Neuropathy (loss of protective sensation)
If you can’t feel pain normally, you keep walking on the wound—pressure keeps damaging it. CDC highlights neuropathy as a major driver of ulcer risk.
Treatment overview by stage (what clinicians typically do)
You’ll see searches like “how to treat diabetic foot ulcer” or “how to heal a diabetic foot ulcer.” I’m not going to give you a DIY protocol—because the wrong home treatment can worsen infection or delay care. Here’s what medical care often focuses on:
Grade 0 (pre-ulcer)
- Removing callus/pressure points
- Shoe/boot changes and offloading
- Daily checks and fast response to any skin break
Grade 1 (superficial ulcer)
- Wound cleaning and appropriate dressings
- Offloading (reducing pressure—this is huge)
- Monitoring for infection signs
Grade 2–3 (deeper ulcer / abscess / bone risk)
- Imaging/labs if infection is suspected
- Debridement (removing dead tissue)
- Antibiotics when infection is present
- Vascular evaluation when circulation looks poor
Grade 4–5 (gangrene)
This is where I stop talking “routine wound care” and start thinking limb—and life—saving. NIDDK states that amputations may be done to prevent severe infection from spreading and to save life.
Can you die from a diabetic foot ulcer?
This is a hard question, but it’s real.
You typically don’t die from the ulcer itself—you die from what it can lead to:
- severe infection spreading to the blood (sepsis),
- uncontrolled tissue death (gangrene),
- delayed care until the body is overwhelmed.
When to go to the ER / call 911

Go to the ER now if you have any of these
- Spreading redness, warmth, swelling around a wound
- Pus/drainage, foul smell
- Fever or chills with a foot wound
- Black tissue or rapidly worsening discoloration
- Increasing pain or (more concerning) no pain with a clearly worsening wound (neuropathy can mask severity)
Call 911 immediately if
- Confusion, collapse, trouble breathing, or signs of severe systemic illness along with a foot infection concern
These can be warning signs of a severe infection affecting the whole body (don’t drive yourself).
How to prevent diabetic foot ulcers
If you searched “how to prevent diabetic foot ulcers,” here are the high-impact basics:
- Check your feet every day
- Don’t ignore calluses, blisters, cracks, or “hot spots”
- Protect feet with well-fitting footwear
- Get foot concerns evaluated early—before it becomes an ulcer or infection
Diabetic foot ulcers don’t usually start “big.” They start small, get missed, then turn serious—especially when there’s neuropathy, poor circulation, or infection. If you’re seeing an open sore, drainage, worsening redness, black tissue, or you’re just not sure how bad it is:
Visit Angleton ER — open 24/7.
Frequently Asked Questions
What are diabetic foot ulcers?
A diabetic foot ulcer is an open sore (often on the bottom of the foot or toes) that happens when diabetes-related nerve damage plus poor circulation makes small injuries easy to miss and slow to heal.
How do diabetic foot ulcers start?
Most start small: a blister from shoes, a cracked heel, a cut, or pressure under a callus. The danger is you may not feel it (neuropathy), so it keeps getting worse until it breaks down into an ulcer.
What does a diabetic foot ulcer look like?
Common signs include an open crater, drainage on socks, surrounding redness/swelling, bad odor, or skin that looks black/gray (possible dead tissue). If you can’t feel your feet well, don’t trust “it doesn’t hurt” as reassurance.
Why do ulcers get worse so fast?
Two big reasons:
Infection (diabetic foot infections can escalate quickly and need prompt clinical management).
Poor blood flow (PAD), which reduces oxygen delivery and slows healing.
How do doctors treat / heal a diabetic foot ulcer?
Treatment depends on stage and infection risk, but commonly includes offloading pressure, proper wound care, removing dead tissue when needed, assessing circulation, and treating infection when present—guided by evidence-based diabetic foot infection recommendations.
I avoid promising a “cure,” because healing depends on depth, circulation, infection, and how quickly care starts.
How can I prevent diabetic foot ulcers?
The highest-impact habits are:
Check your feet daily for cuts, redness, swelling, sores, blisters, corns, or calluses.
Don’t try to remove corns/calluses yourself.
Get routine foot checks—especially if you’ve had ulcers or neuropathy symptoms.
Can you die from a diabetic foot ulcer?
Not from the ulcer by itself—but from what it can lead to: severe infection spreading (including life-threatening complications) or extensive tissue death. NIDDK explicitly notes amputations may be done to prevent infection from spreading and to save your life.
Which “stage” should be treated as urgent?
If the ulcer is deep (tendon/joint/bone risk), has abscess/osteomyelitis concern, or any gangrene is present, it’s urgent. Wagner grades 3–5 reflect those higher-risk categories and need immediate medical attention.