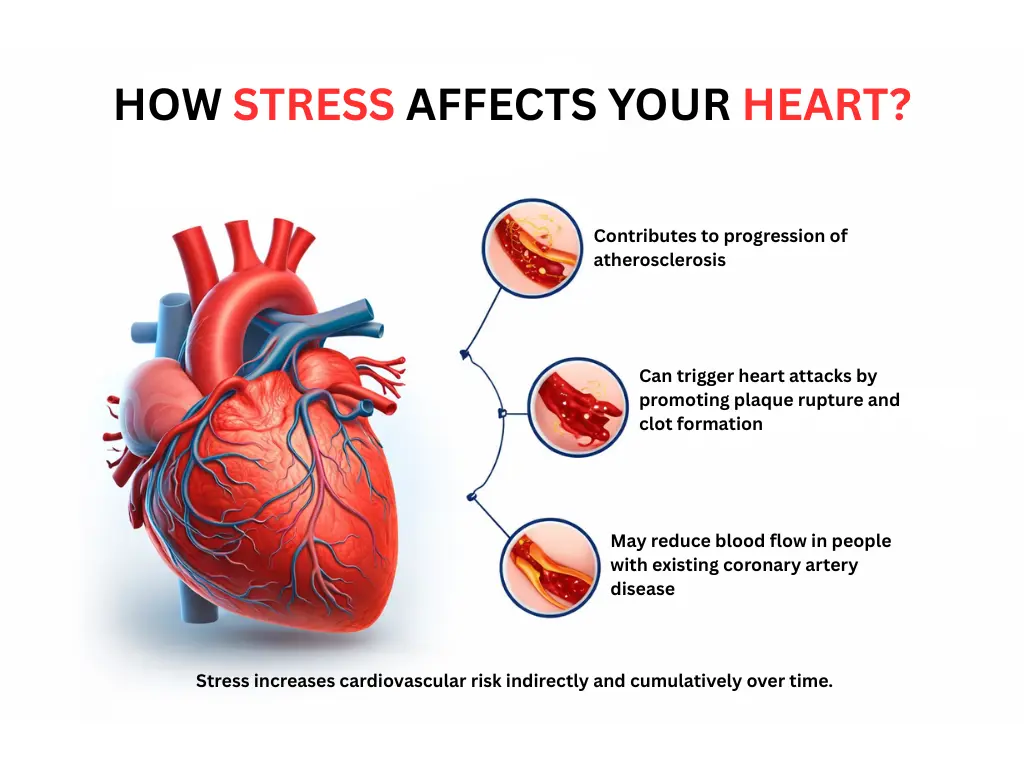
If you’re here because your chest feels tight, your heart feels like it’s racing, or you keep thinking, “Is stress doing something to my heart?” — you’re not alone. We see this worry all the time, and it’s a reasonable question.
Here’s the honest, doctor-style answer: yes, stress can cause real physical heart symptoms. Sometimes it’s your body’s “alarm system” (adrenaline) doing exactly what it was designed to do. And sometimes, those symptoms overlap with real heart problems — which is why we don’t guess from the couch.
(Anonymous scenario, because this is common: A patient comes in after a brutal week — poor sleep, nonstop deadlines, family stress. They feel chest tightness and a pounding heartbeat out of nowhere. They’re scared it’s a heart attack. After an evaluation, the picture fits a stress/anxiety surge — but the most important part is this: they didn’t “waste a trip.” They got clarity, safely.)
Quick answer
Can stress cause heart problems? Yes — in a few different ways.
- Stress can trigger symptoms like a racing heart, pounding heartbeat, chest tightness, and shortness of breath sensations.
- Stress can worsen existing heart conditions by increasing strain on the cardiovascular system.
- Chronic stress can raise long-term risk indirectly by pushing blood pressure up and driving coping habits that hurt heart health (poor sleep, smoking, alcohol, inactivity, overeating).
- But stress symptoms and heart symptoms can look alike. When the symptoms are new, intense, or concerning — we recommend evaluation rather than self-diagnosis.
What stress can do to your body (the “adrenaline effect”)
When you’re under stress, your nervous system can flip into fight-or-flight mode. That can cause:
- Faster heart rate or a pounding heartbeat
- Chest tightness or a “heavy” feeling in the chest
- Shortness of breath sensation (sometimes from breathing faster or shallower)
- Sweating, nausea, shakiness
- Tingling in hands/around the mouth (often from over-breathing)
- Feeling detached, dizzy, or “not right”
But the adrenaline surge doesn’t just stop at physical symptoms. Chronic stress can stir up a whole collection of emotional and mental symptoms too—like irritability, anxiety, depression, rumination, and trouble sleeping (including waking up in the middle of the night with your mind racing). Sometimes, it’s not just your heart that feels the strain; it’s your mood, your sleep, and your ability to shake off worries.
These symptoms are real. They’re not “in your head.” But they don’t automatically mean you’re having a heart attack, either.
A practical way to think about it: stress can make your body act like it’s running from danger — even if the danger is an email, an argument, or a week of poor sleep.
When stress actually helps: The upside of “fight-or-flight”
It’s easy to paint stress as the villain, but—believe it or not—short bursts of stress can sometimes be an asset. Think of it as your body’s internal “turbo mode.” Adrenaline ramps up when you need to ace that big presentation, power through final exams, or swerve quickly to avoid a fender-bender.
These short-term stress spikes can:
- Sharpen your focus, so you solve problems faster.
- Give you a temporary energy surge to meet tight deadlines or face difficult conversations.
- Boost alertness and memory, so you remember details right when you need them.
In essence, a healthy jolt of stress can help you rise to the occasion—whether that’s acing a job interview, getting through your busiest shift of the year, or just sprinting to catch your connecting flight at O’Hare. The trouble comes when that same stress response is switched on all the time. That’s when the helpful adrenaline rush starts to work against you…and your heart.
Can anxiety cause heart problems?
People ask this in two ways:
1) “Can anxiety cause heart symptoms?”
Yes. Anxiety can cause heart-centered symptoms — palpitations, chest tightness, shortness of breath feelings — because anxiety activates the same fight-or-flight system.
2) “Can anxiety damage my heart?”
Most of the time, anxiety itself is not “damaging the heart” in a direct way. The bigger issue is this: if anxiety (or chronic stress) drives high blood pressure, poor sleep, smoking, alcohol, or inactivity over time, those patterns can increase cardiovascular risk.
So we take anxiety seriously for two reasons:
- It can feel terrifying and disruptive.
- It can overlap with real heart problems — and you deserve clarity, not dismissal.
Is it anxiety or heart problems? How we think through it
There’s no perfect at-home checklist that can safely rule out heart issues. But there are patterns that help guide what to do next.
Patterns that often lean “stress/anxiety surge”
These can still be miserable — but they often show up like:
- Symptoms come on during or after an obvious stress spike (conflict, panic, bad news, caffeine + no sleep)
- Racing heart + shakiness + sweating + tingling all together
- A strong sense of fear or doom paired with physical symptoms
- Symptoms improve when you can slow your breathing, change environment, or get reassurance
- Symptoms come in waves (peaks and falls)
Even if your symptoms “sound like anxiety,” we don’t recommend assuming. Especially if it’s new for you.
Patterns that deserve medical evaluation
These are the ones we take seriously right away, because they can point to heart or lung emergencies:
- Chest pressure, squeezing, or heaviness that doesn’t settle
- Shortness of breath that’s new or worsening
- Fainting or near-fainting
- Chest discomfort plus sweating, nausea, or weakness
- Pain that spreads to the arm, shoulder, jaw, neck, or back
- Symptoms that come on with exertion (walking, climbing stairs)
- A known history of heart disease, uncontrolled high blood pressure, diabetes, kidney disease, or significant risk factors
If you’re unsure which bucket you’re in, that uncertainty itself is a good reason to get evaluated.
Long-term: can stress increase cardiovascular risk?
This is where stress matters even when you’re not having dramatic symptoms.
Chronic stress can contribute to heart risk in two main ways:
- Physiology: Stress hormones can affect blood pressure and inflammation pathways.
- Behavior loops: Stress often pushes people toward habits that raise risk — poor sleep, less activity, smoking/vaping, alcohol, comfort eating, missed medications, or skipping routine care.
But it’s not all doom and gloom. Easing stress isn’t about flipping a switch—it’s about building realistic routines that support both your mood and your heart. One of the simplest (yet most overlooked) tools? Physical activity. Regular exercise doesn’t just help your headspace—it actively lowers blood pressure and helps combat other cardiovascular risk factors, like high cholesterol and weight gain. And you don’t have to turn into a gym rat: even a brisk walk, a dance around the kitchen, or a few flights of stairs can make a difference.
So if you’ve been under sustained stress for months, the goal isn’t to be “perfect.” It’s to be realistic:
- prioritize sleep where you can
- reduce nicotine and heavy alcohol
- move your body most days (even short walks)
- keep blood pressure and diabetes care consistent
- talk to a clinician if anxiety is running your life
That’s heart care too.
What if stress or low mood just won’t budge?
If you find yourself stuck in a loop of constant stress or low mood that doesn’t seem to let up, you’re not alone—and you don’t need to tough it out by yourself. Reaching out to a mental health professional—whether that’s your primary care doctor, a therapist, or even support lines from reputable organizations like the National Alliance on Mental Illness (NAMI)—can be a crucial step. Just as we take heart symptoms seriously, persistent stress or depression deserves real attention and support. It’s a sign of strength, not weakness, to ask for help.
Does attitude matter? Finding the “silver lining”
It might sound like something from a self-help book, but there’s real value in how we approach stress. Spotting the “silver lining” or practicing a positive outlook isn’t about ignoring real problems—it’s about training your brain to respond differently when they show up.
Here’s why this matters:
- Focusing on what’s in your control (instead of spiraling about what isn’t) can lower stress hormone spikes.
- Finding small moments of calm—even when life is messy—helps your body recover from tension faster.
- Over time, people who nurture a more hopeful or accepting mindset tend to report lower stress and a better quality of life, even if their external circumstances don’t change overnight.
No one needs to be relentlessly cheerful. But pausing to notice good moments, reframing challenges, or just cutting yourself some slack are all proven ways to turn down the stress dial—and that helps your heart and your overall well-being.
What about mindfulness, meditation, and yoga?
These tools aren’t just for people who own Himalayan salt lamps. Practices like mindfulness, meditation, and yoga can help dial down the body’s stress response—sending a clear “stand down” message to your fight-or-flight system.
- Mindfulness and meditation: Even a few minutes a day can help calm racing thoughts, slow your breathing, and lower stress hormones. Headspace, Calm, or even a quiet corner and a YouTube video can get you started—no incense required.
- Yoga: Whether it’s a Power Yoga flow or a simple series of stretches, yoga blends movement, focused breathing, and moments of pause. Studies suggest it helps lower stress, improve mood, and may even benefit blood pressure over time.
The bottom line: you don’t need to become a guru—adding even small doses of these practices can help smooth those stress peaks and support your heart in the long run.
The Real-World Toll of Workplace Stress
Zoom out from individual habits, and there’s no denying the collective impact of workplace stress on both well-being and productivity. Most folks spend a huge chunk of their waking hours on the job — and for many, that’s where stress first ramps up. In fact, surveys by organizations like the American Psychological Association routinely show that nearly two-thirds of workers point to their jobs as a top source of stress.
What actually happens when job-related stress piles on?
- Creativity and productivity take a hit: High-stress environments sap focus, stifle fresh ideas, and make problems harder to solve.
- Absences go up: Burnout and chronic stress feed into more sick days, whether for mental health or the physical effects of stress.
- Real dollars at stake: Studies out of Harvard and Stanford suggest that annual costs linked to workplace stress — from lost output to extra healthcare needs — run into the hundreds of billions nationally each year.
Whether it’s long hours, job insecurity, heavy workloads, or physical strain, these stressors don’t just vanish at the end of the workday. Over time, they ripple out, influencing everything from sleep quality to blood pressure to relationships at home.
Left unchecked, chronic stress at work can sow the seeds for both mental and heart health struggles down the line. That’s why taking steps to manage workplace pressure isn’t fluff — it’s a genuine investment in your health.
How to test heart problems
When someone comes in with chest symptoms, racing heart, or “I feel like something’s wrong,” we’re not trying to win an argument with anxiety — we’re trying to answer one question:
Is there evidence of a dangerous heart (or lung) problem right now?
Here are common tools clinicians use, depending on symptoms:
Does an EKG show heart problems?
An EKG (ECG) can show patterns that suggest:
- heart rhythm problems
- heart strain
- signs that may point toward reduced blood flow to the heart
But an EKG is not a crystal ball. A normal EKG doesn’t automatically mean “nothing is wrong,” and an abnormal EKG doesn’t automatically mean “heart attack.” It’s one piece of the puzzle.
(This is why “does an EKG show heart problems?” is a fair question — and the honest answer is: sometimes it helps a lot, but it’s not the only test.)
Can a blood test detect heart problems?
Sometimes, yes. Blood tests can look for signals of heart muscle stress or injury. One well-known example is troponin, which can rise when there’s heart muscle injury.
But blood tests are also not “one test that solves everything.” They must be interpreted in context:
- your symptoms
- your exam
- the EKG
- timing and overall risk
So if you’re thinking: “can blood test show heart problems?” — the doctor answer is: it can help, but it’s part of a bigger picture.
Can a chest X-ray show heart problems?
A chest X-ray doesn’t diagnose coronary artery disease. But it can be useful for related problems that cause chest symptoms, such as:
- certain lung conditions
- fluid patterns that may fit heart strain
- other non-heart causes of chest discomfort
What else might be considered?
Depending on your situation, clinicians may also consider:
- additional cardiac monitoring (watching rhythm over time)
- ultrasound imaging (for specific questions)
- outpatient follow-up testing (like stress testing) when appropriate
Bottom line: testing is about ruling in/out dangerous causes and guiding next steps — not labeling every symptom as “anxiety” or “heart disease” without evidence.
What you can do in the moment (if symptoms are mild and you’re not in the “shouldn’t wait” bucket)
If symptoms are mild and you’re not having warning symptoms that shouldn’t wait, these are reasonable, low-risk steps that often help stress-driven symptoms:
- Slow your breathing: inhale gently through the nose, longer exhale through the mouth
- Cut caffeine for the day (especially energy drinks)
- Hydrate and eat something light if you haven’t eaten
- Change the input: step outside, sit upright, loosen tight clothing
- Name the pattern: “My body is in alarm mode. I’m safe while I assess what’s happening.”
If symptoms persist, recur, or escalate — get evaluated. The goal is safety first, pride last.
Warning symptoms that shouldn’t wait
If you have any of the following, it’s reasonable to seek urgent evaluation:
- Chest pressure, squeezing, heaviness, or pain that is new, intense, or not improving
- Shortness of breath that’s new, worsening, or happening at rest
- Fainting, near-fainting, or sudden severe dizziness
- Chest discomfort plus sweating, nausea/vomiting, or unusual weakness
- Pain spreading to the arm, shoulder, jaw, neck, or back
- A new irregular heartbeat feeling with weakness, chest discomfort, or shortness of breath
- Symptoms that occur with exertion (walking, stairs)
- You “just feel wrong” in a way that’s hard to explain — especially if it’s new for you
If you’re debating it, that’s often your cue: don’t talk yourself out of care.
If you’re experiencing chest discomfort, shortness of breath, fainting/near-fainting, or symptoms that feel concerning — and you’re in or near Angleton or surrounding Brazoria County communities — it’s reasonable to get evaluated. At Angleton ER, we’re open 24/7, and our team can help assess heart- and chest-related symptoms with on-site diagnostics when needed.
Frequently Asked Questions
Can stress cause heart problems even if I’m healthy?
It can cause real symptoms even in otherwise healthy people — especially palpitations, chest tightness, and shortness-of-breath sensations. The key is whether symptoms are new, severe, or paired with warning symptoms that shouldn’t wait.
Does stress cause heart problems like a heart attack?
Stress alone is not usually the sole cause, but stress can increase strain on the body and may contribute to risk over time. If symptoms feel like a heart attack — don’t guess. Get evaluated.
Can anxiety cause heart problems, or just mimic them?
Anxiety can absolutely mimic heart problems. And chronic anxiety/stress can contribute to risk indirectly by affecting sleep, blood pressure, activity, and coping behaviors. Either way, you deserve a real assessment if symptoms are concerning.
Is it anxiety or heart problems if my chest feels tight?
It could be either — and sometimes both are playing a role. Tight chest + fear can happen with panic, but chest tightness can also happen with heart and lung issues. If it’s new, worsening, or paired with warning symptoms that shouldn’t wait, get checked.
How to test heart problems when symptoms come and go?
Clinicians often use a combination of EKG, blood tests, and sometimes imaging/monitoring, depending on your symptoms and risk. Intermittent symptoms can still be evaluated — especially if they’re recurring or escalating.
Can a blood test detect heart problems?
A blood test can sometimes detect signs of heart muscle stress or injury (for example, troponin). It’s interpreted alongside symptoms and other tests.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.