Yes — you can absolutely have neuropathy without diabetes.
In the ER, I meet plenty of people around Angleton and nearby Brazoria County communities (Lake Jackson, Clute, Alvin) who assume numbness or burning in the feet must mean diabetes. Diabetes is a common cause, but it’s not the only one. ( Angleton’s 2024 population estimate is 20,979, and 19.1% of residents are 65+, which matters because neuropathy risk rises with age and other health conditions.)
Below, I’ll walk you through what neuropathy feels like, common non-diabetes causes, how we sort out whether diabetes is involved, and when symptoms become an ER or 911 situation.
Quick answer
Neuropathy means nerve damage. It can be caused by diabetes, but also by vitamin problems, alcohol, toxins, certain medications, infections, autoimmune issues, nerve compression, and kidney/liver disease — among other causes.
What neuropathy feels like
Most people describe neuropathy as:
- Tingling (“pins and needles”)
- Numbness or reduced sensation
- Burning pain
- Sharp, stabbing, or electric shocks
- Sensitivity to touch
- Weakness or poor balance
Mayo Clinic notes symptoms often start in the hands or feet and can include numbness, tingling, burning, sharp pain, and weakness.
What does diabetic neuropathy feel like?
Diabetes-related peripheral nerve damage usually starts in the feet and can cause tingling, pain (often worse at night), numbness, weakness, and serious foot complications.
If you’re wondering “what are the 5 main symptoms of diabetic neuropathy?”: tingling, burning/pain, numbness, weakness, and increased sensitivity (often in the feet) are the big ones I see—especially when it’s progressing.
Does diabetic neuropathy come and go?
It can. Early symptoms sometimes fluctuate, especially when inflammation, activity level, footwear, hydration, and blood sugar control vary—but persistent or worsening symptoms should be evaluated.
Common causes of neuropathy without diabetes
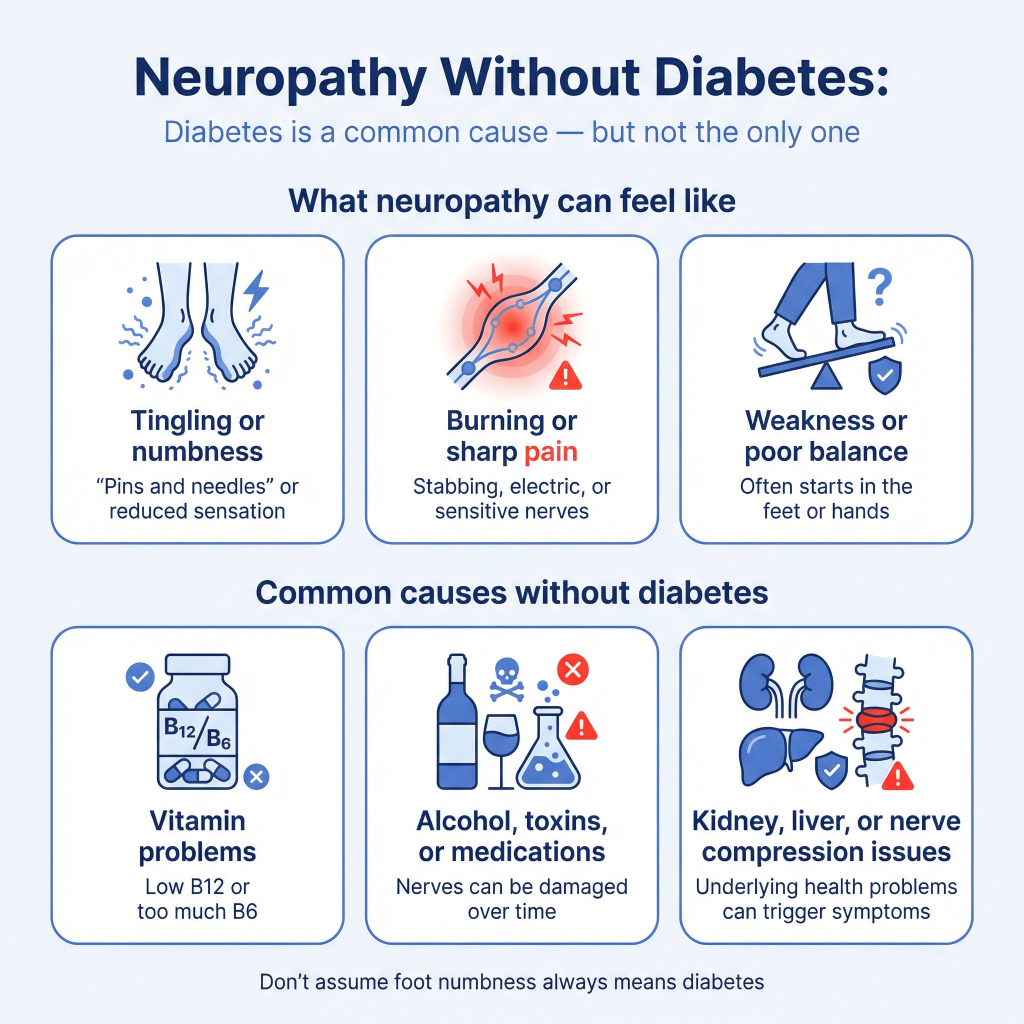
Here are causes I see regularly in people without diabetes (or before diabetes is ever confirmed):
Vitamin or nutrition problems
The National Institute of Neurological Disorders and Stroke specifically calls out:
- Vitamin B12 deficiency
- Excess vitamin B6
as well-known vitamin-related causes of neuropathy.
Alcohol use
NINDS notes alcoholism can damage nerves and cause neuropathy.
Toxin exposure
NINDS also lists exposure to toxins as a cause.
Kidney or liver disease
When kidneys or liver don’t clear toxins well, those toxins can injure nerve tissue. NINDS explains kidney and liver disorders can raise toxin levels in the blood and damage nerves.
Nerve compression or injuries
Pinched nerves, repetitive stress, spine issues, or physical injury can cause neuropathy-like symptoms. MedlinePlus explains peripheral nerve disorders happen when peripheral nerves are damaged; causes vary widely.
Other medical causes
How I tell if neuropathy is from diabetes
This is where many people get stuck. Here’s the practical truth:
- Diabetes is common, so we consider it early.
- But we don’t assume it’s diabetes just because symptoms are in the feet.
Mayo Clinic notes peripheral neuropathy has many causes and evaluation typically includes a physical exam and often blood tests as part of figuring out the cause.
CDC explains diabetes-related peripheral nerve damage often starts in the feet and is associated with sensory symptoms and foot complications.
What tests and exams doctors use
You’ll often hear about “neuropathy testing,” but some of the most useful checks are basic:
A focused nerve exam
Clinicians check sensation, strength, reflexes, balance, and areas where numbness starts or spreads.
Monofilament testing
(This directly answers the question: “what is being tested with a monofilament for diabetic neuropathy?” — it’s testing protective sensation / large fiber function that correlates with foot-ulcer risk.)
Who treats neuropathy?
A lot depends on what’s driving it:
- Primary care often starts the evaluation (labs, medication review, risk factors).
- Neurology may be involved for persistent, unclear, or progressive cases.
- Podiatry can be crucial when symptoms affect the feet, balance, or wound risk.
Mayo Clinic emphasizes early evaluation and individualized workup because causes vary.
Is diabetic neuropathy reversible? Can you reverse diabetic neuropathy?
Here’s the honest medical answer:
- Some people see improvement in symptoms when the underlying driver is addressed (like better glucose control, correcting vitamin issues, stopping toxins, etc.).
- But nerve damage can also be partial or permanent, especially if it’s advanced or has been present a long time.
Mayo Clinic’s treatment approach focuses on addressing underlying causes and symptom control—because outcomes depend on the cause and severity.
So when someone asks “how to cure diabetic neuropathy” or “how to reverse diabetic neuropathy”: I frame it as treat the cause + protect the feet + manage pain + prevent progression, not a guaranteed “cure.”
When to go to the ER or call 911
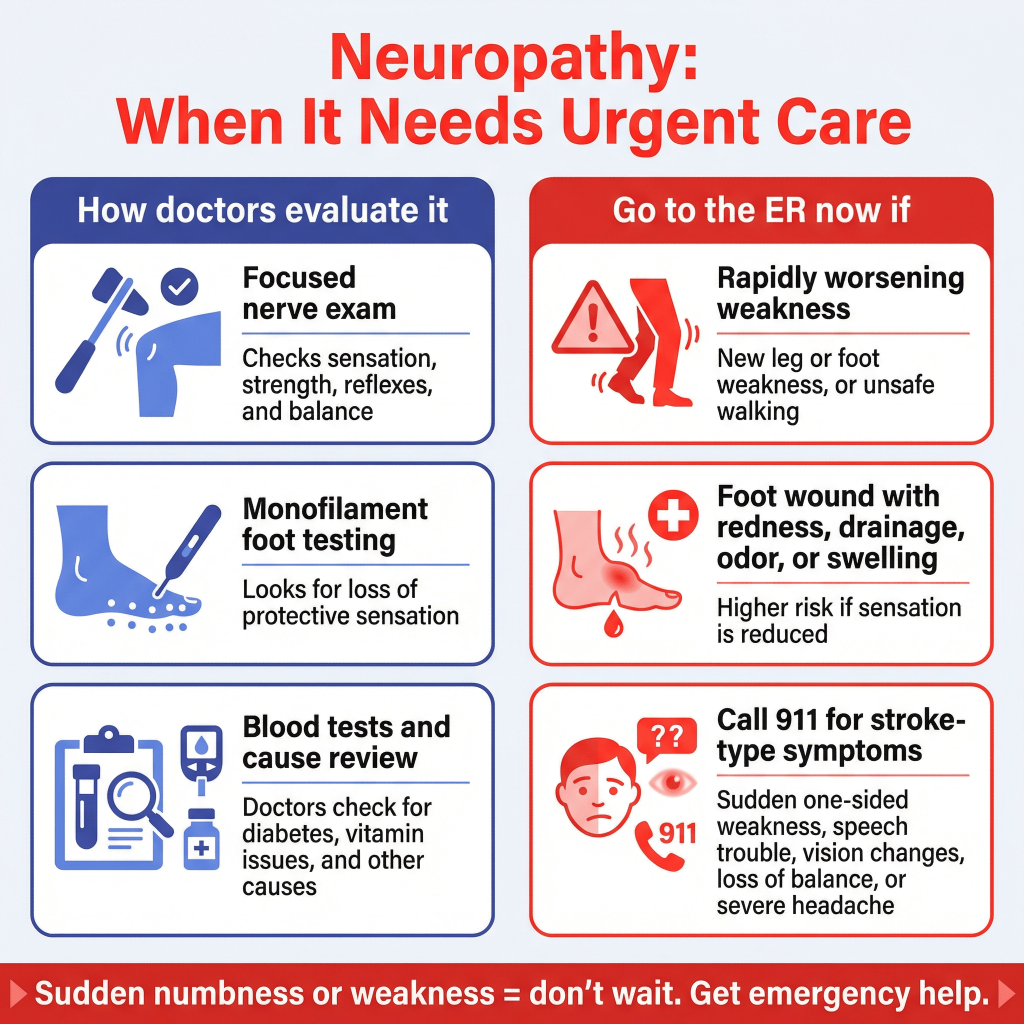
Neuropathy is often not an emergency—but certain patterns absolutely are.
Go to the ER now if
- You develop new, rapidly worsening weakness in a leg/foot or can’t walk safely
- You have a foot wound, spreading redness, drainage, bad odor, or severe swelling (especially if you have decreased sensation)
- You have fever with a painful or red/swollen foot
- You have severe pain that’s out of control or symptoms that are escalating quickly
CDC notes diabetes-related nerve damage can lead to serious foot problems like ulcers and infections.
Mayo Clinic advises seeking medical care right away for unusual tingling, weakness, or pain in the hands or feet—early evaluation helps prevent further nerve damage.
Call 911 immediately if
If symptoms are sudden, think stroke until proven otherwise:
- Sudden numbness or weakness of face/arm/leg, especially on one side
- Sudden confusion, trouble speaking or understanding speech
- Sudden trouble seeing
- Sudden trouble walking, dizziness, loss of balance
- Sudden severe headache with no known cause
If you’re feeling numbness, tingling, burning pain, or weakness—don’t assume it’s diabetes, but also don’t ignore it. Neuropathy has many causes, and the sooner you identify the real one, the better your chances of protecting your nerves and your mobility.
Visit Angleton ER — open 24/7.
Frequently Asked Questions
What causes diabetic neuropathy?
Diabetes-related nerve damage is commonly associated with long-term high blood sugar and often begins in the feet, causing tingling, pain, numbness, and weakness.
How long does diabetic neuropathy take to develop?
It varies widely. Some people develop symptoms earlier, others later—risk increases with longer duration and poor glucose control. The key is early evaluation when symptoms begin.
How to treat diabetic neuropathy / how do you treat diabetic neuropathy?
Treatment typically focuses on managing the underlying cause and controlling symptoms. Mayo Clinic describes treatment as addressing underlying causes and symptom management (often pain control and function protection).
Is diabetic neuropathy fatal?
Neuropathy itself isn’t typically “fatal,” but it can contribute to serious complications (like unnoticed foot wounds leading to severe infection). That’s why prevention and early care matter.

