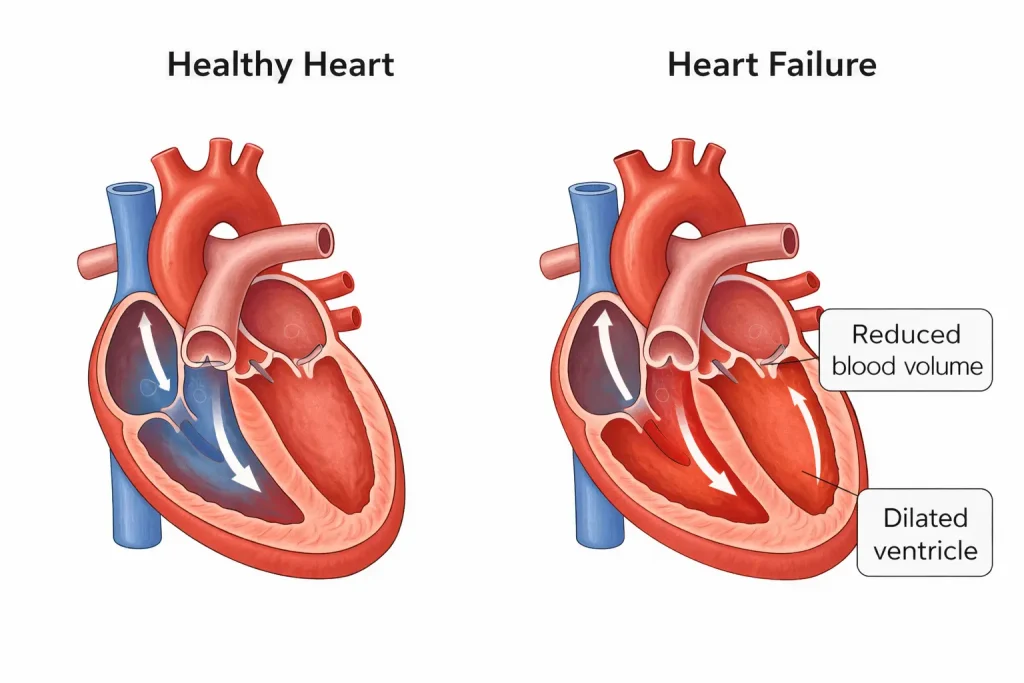
If you searched “what is congestive heart failure”, there’s a good chance you’re not doing it out of curiosity. Most people end up here because something feels off — a new diagnosis, a scary symptom, or a loved one using the words “heart failure” like a sentence.
Let us start with the part we say out loud in the ER all the time:
Heart failure does not mean your heart has stopped. It also doesn’t mean you did something wrong. It means the heart isn’t keeping up with the body’s needs the way it should — and because blood flow and fluid balance are connected, symptoms can show up in ways that feel confusing and honestly pretty frightening.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.
The first thing most people misunderstand about CHF
When people hear “congestive heart failure,” they picture a heart that’s about to quit. That’s not how we think about it clinically.
CHF is less about a sudden “failure” and more about a system that’s under strain:
- the heart isn’t pumping efficiently enough, and/or
- it isn’t filling efficiently enough, and/or
- the body is holding onto fluid in ways that create congestion.
That congestion is where many symptoms come from: fluid that backs up toward the lungs, swelling in the legs, a feeling of heaviness, fatigue that doesn’t match what you did that day.
We also want to say this plainly: CHF can be serious, but it’s also often treatable and manageable, especially when the cause is addressed and symptoms are recognized early.
A quick anonymous scenario
A patient comes in from Brazoria County because they’ve been “getting winded” doing normal things — walking from the car, climbing a few steps, laying down at night. They tell us they’ve also noticed their shoes feel tighter and their legs look puffier at the end of the day.
They’re not trying to diagnose themselves. They’re trying to answer one question:
“Is this something I can watch… or something I shouldn’t ignore?”
That’s a fair question. In the ER, our job is to make sure we’re not missing the time-sensitive, dangerous causes — and then to help connect the symptoms to what’s actually happening inside the body.
What congestive heart failure actually means
“Heart failure” is an umbrella term. “Congestive” points to the fluid backup part.
the heart isn’t moving blood forward as effectively as it should, and the body can respond by holding onto fluid. That fluid can build up:
- in the lungs (making breathing harder),
- in the legs/ankles (swelling),
- in the abdomen (bloating, reduced appetite),
- sometimes even as a general “puffy” feeling.
What does each stage (A, B, C, D) of congestive heart failure mean?
Heart failure doesn’t happen all at once; it often moves through stages—long before any swelling or shortness of breath ever shows up. Understanding where someone falls can help make sense of what to expect, and why prevention or early attention matters.
Let’s walk through the stages the way we would explain it to someone in clinic, using the framework the American Heart Association and American College of Cardiology use—the ABCDs of heart failure:
Stage A: The “risk factors, but no damage yet” group
This stage isn’t heart failure itself. Instead, it includes people who have conditions that raise the risk of developing heart failure down the road. Think high blood pressure, diabetes, a strong family history of heart trouble, metabolic syndrome, heavy alcohol use, or a past diagnosis of rheumatic fever. Here, the heart is still ticking along, but there’s enough risk in the picture that prevention is key.
Stage B: Structural changes, but no symptoms
Stage B is a little like finding a pothole on the road before you’ve gotten a flat tire. The heart shows changes on imaging—maybe a weak left ventricle or another structural issue—but the person hasn’t felt a thing yet. This is the “quiet phase”: signs are there behind the scenes, but daily life usually feels normal.
Stage C: Symptoms, either now or in the past
Now we’re in territory where things get noticeable. Stage C means someone has evidence of heart failure and has either experienced symptoms (like swelling, breathlessness, or fatigue) or still deals with them off and on. This is often where the diagnosis first gets made, because the body is sounding the alarm in obvious ways.
Stage D: Advanced or refractory symptoms
Stage D is the “we’ve tried everything” stage. Here, symptoms are persistent and resist standard therapies—breathing remains tough, swelling sticks around, and options like advanced treatments or even transplant come onto the table. It’s the most serious stage, and it generally means the heart is struggling despite best medical efforts.
These stages help guide not just what we watch for, but how aggressive we get with treatment or prevention.
The four stages of congestive heart failure
If you’ve ever wondered how heart failure is “graded,” here’s how doctors break it down in practice. CHF isn’t an all-or-nothing diagnosis—it’s a spectrum, with four main stages:
Stage A: At risk, but no damage yet
This covers folks who don’t have symptoms or structural heart issues but are walking around with risk factors—think high blood pressure, diabetes, a family history of heart failure, taking certain cancer medications, or a history of heavy alcohol use. The heart is still doing its job, but the dominos are lined up.
Stage B: The heart has changed, but you don’t notice
At this point, the heart muscle or structure isn’t quite normal—maybe from a prior heart attack or valve problem—but you don’t feel symptoms yet. It’s like the warning light is on, but nothing’s sputtering yet.
Stage C: Heart failure symptoms, now or in the past
Here’s where signs of CHF become recognizable: breathlessness, swelling, fatigue, or all of the above. Whether you have symptoms right now or have had them before, Stage C means the diagnosis moves from “theoretical” to “real life.”
Stage D: Symptoms despite everything
This is advanced heart failure: symptoms that are severe or don’t improve even with treatments like medications and lifestyle changes. People in this stage may find themselves short of breath at rest, struggling with swelling that won’t budge, or needing frequent hospital visits.
Most important: plenty of people never progress past the early stages—especially if risks are managed early and triggers are addressed. But knowing your stage can help guide the next steps, whether that’s prevention, starting meds, or considering advanced therapies.
What are the types of congestive heart failure?
Just like “congestion” describes fluid backing up in places it shouldn’t, the label “heart failure” gets divided into a few different types depending on which part of the heart is struggling and how the body is reacting.
Here’s a quick breakdown:
- Left-sided heart failure: This is the most common form. The left side of the heart can’t keep up—either because it can’t squeeze strongly enough (systolic) or can’t relax enough to fill (diastolic). This can lead to fluid backing up toward the lungs, making breathing harder.
- Right-sided heart failure: Here, the right side of the heart is the main culprit. When it isn’t pumping well, fluid can collect in the body—especially in the legs, ankles, and sometimes the belly—causing swelling and a heavy, tired feeling.
- High-output heart failure: Less common, but worth mentioning. In this scenario, the heart is working harder than usual but still can’t meet the body’s needs. This can be triggered by conditions like severe anemia or overactive thyroid, and it doesn’t look exactly like the classic “weak heart muscle” picture.
Most people fit into one of the first two buckets—or a mix—but knowing the type helps guide both treatment and what symptoms to watch for.
How common is congestive heart failure?
You’re not alone if you—or someone you care about—has been told they have CHF. In fact, heart failure is surprisingly common. Millions of Americans live with it every day, and it’s actually one of the most frequent reasons older adults end up in the hospital. While the numbers grow as people age, it touches families in nearly every community regardless of background. It’s a big part of why so much attention is focused on early recognition, better treatments, and making sure people know what symptoms to look for.
Why symptoms vary so much
Two people can both have CHF and describe completely different experiences:
- one mainly feels short of breath,
- another mainly notices swelling and weight changes,
- another feels fatigue and can’t explain why they “just can’t get going.”
That’s why “CHF” isn’t a symptom — it’s a framework for understanding why symptoms cluster together.
It’s also important to know that symptoms can range from barely noticeable to hard-to-ignore, and they might come and go. Some people with CHF have very mild symptoms, or even none at all, at certain times. This doesn’t mean the heart failure has gone away—just that it isn’t always obvious or severe every day.
This variability is part of what makes CHF tricky: the same condition can look very different from one person to the next, or even from one day to another.
What CHF can feel like in real life
This section matters because most people don’t show up saying, “I think I have heart failure.” They show up describing how their day-to-day has changed.
Breathing changes (the most common reason people come in)
Some people notice:
- they’re short of breath with less activity than usual,
- they can’t lie flat comfortably,
- they wake up at night feeling like they need to sit up to breathe,
- they feel “air hungry,” even if they’re not wheezing.
Not all shortness of breath is CHF — lung infections, asthma/COPD, anxiety, blood clots, and other conditions can overlap. But if breathing changes are new, worsening, or don’t match your normal, we take that seriously.
Fatigue that feels disproportionate
Heart failure fatigue often gets described as:
- “I’m tired, but it’s not sleep tired.”
- “I’m wiped out doing normal stuff.”
- “My body feels heavy.”
Again — fatigue has many causes. What matters is change: new fatigue, rapidly worsening fatigue, or fatigue with other symptoms like swelling or shortness of breath.
Swelling (legs, ankles, sometimes abdomen)
Swelling may show up as:
- sock lines that suddenly leave deeper marks,
- shoes that feel tight at the end of the day,
- ankles that look puffy,
- rings that feel tighter.
Swelling can also come from non-heart causes (kidney issues, liver issues, certain medications, vein problems). But when swelling pairs with breathing changes or unusual fatigue, we think broader and move faster.
Cough or “chest congestion”
Some people notice a persistent cough, especially if fluid is backing up toward the lungs. This can be mistaken for allergies or a lingering cold — and sometimes it really is. But if a cough is paired with shortness of breath, worsening swelling, or sudden exercise intolerance, it deserves a closer look.
What causes CHF (how we think about it clinically)
People ask “what causes congestive heart failure” because they want the “why.” That’s reasonable.
In the ER and in cardiology, we usually think in buckets:
1) Long-term strain on the heart
Conditions like high blood pressure can force the heart to work harder over time. The heart muscle may change — thickening or stiffening — and that can contribute to CHF symptoms.
But it’s not just blood pressure. Risk factors that put long-term strain on the heart (even before symptoms start) include:
- Being older than 65
- Having an inactive (sedentary) lifestyle
- Eating foods high in salt and fat
2) Damage to the heart muscle
Sometimes the heart muscle is weakened or injured by:
- reduced blood flow to the heart (for example, coronary artery disease),
- inflammation of the heart muscle,
- certain toxins (including heavy alcohol use in some cases),
- other medical conditions that affect the heart over time.
Other contributors in this bucket include:
- Having a heart attack (which directly damages heart muscle)
- Using tobacco products or cocaine (which can injure the heart)
- Having a family history of heart problems
3) Rhythm problems
Some rhythm issues can make the heart beat too fast or irregularly for long stretches, which can contribute to failure symptoms or flare-ups.
4) A “trigger” that tips someone over the edge
Even if CHF is already present, symptoms often worsen because something changed, such as:
- a respiratory infection,
- medication changes,
- missed doses of prescribed medications,
- fluid or salt shifts,
- other stressors on the body.
We’re not saying this to put responsibility on the patient. We’re saying it because identifying triggers often helps prevent repeat flare-ups.
CHF is rarely about just one thing. Age, genetics, lifestyle, blood pressure, heart attacks, and daily choices all play a role. Some people find themselves at the crossroads of several risk factors at once — which is why understanding your own mix of risks can help guide prevention and treatment.
How CHF is diagnosed (what each step is trying to answer)
A big reason people search “how is congestive heart failure diagnosed” is because they want certainty. We get that.
Diagnosis isn’t usually one magic test. It’s a combination of:
- symptoms,
- exam findings,
- and tests that point toward (or away from) fluid overload and heart strain.
Step 1: History + exam
We listen for clues in your story:
- What changed?
- How fast did it change?
- What makes it better or worse?
We also look for physical signs of congestion or strain — breathing pattern, swelling, oxygen needs, heart rhythm, lung sounds.
Step 2: EKG (ECG)
An EKG is very useful for rhythm problems and signs that the heart is under stress. But an EKG alone usually does not “prove” CHF. What it can do is help us spot problems that may be connected to symptoms or that need urgent attention.
Step 3: Blood tests (high-level, no “numbers online”)
There are blood tests that can support the picture of heart strain and fluid overload — but they need to be interpreted in context. Other tests help us evaluate kidney function, infection, anemia, and other contributors to symptoms.
Step 4: Chest imaging and heart imaging
Depending on the situation, imaging can help us assess lungs, fluid patterns, and other causes of shortness of breath. An echocardiogram (ultrasound of the heart) is often used to better understand how the heart is pumping and filling.
Key point: If you’re trying to self-diagnose from one result — an EKG, one lab, one scan — that’s where misinformation spreads. CHF is a clinical picture, and context matters.
How CHF is treated (and what’s safe to do right now)
People also search “how to treat congestive heart failure” because they want a plan, not a lecture.
Treatment usually focuses on two goals:
- Relieve congestion and reduce strain (help you breathe easier, reduce swelling, stabilize the system)
- Address the cause and reduce flare-ups (long-term risk reduction and stability)
Relieving congestion
Many treatment plans include medications that help the body get rid of excess fluid and reduce the workload on the heart. The “right” plan depends on why CHF is happening and what other conditions are present.
Adjusting your diet: Salt and fluid matters
With congestive heart failure, tweaking what you eat and drink isn’t about punishment—it’s about helping your heart do its job with less strain. For most people, that means watching both salt and fluid intake.
- Salt (sodium): Too much salt makes your body hold onto water, which can worsen swelling and breathing problems. Many clinicians recommend cutting back on added salt and looking out for hidden sodium in packaged or restaurant foods. Even “healthy”-sounding brands can sneak in a surprising amount.
- Fluid: For some, limiting daily fluids can help prevent fluid buildup. The specifics aren’t one-size-fits-all; some people need to be strict, while others have more flexibility, depending on their symptoms and other health factors.
Your clinician can give you personal targets and talk through what these limits actually look like, so you’re not left guessing or relying on random online charts. This isn’t about making life taste bland—it’s about setting you up for fewer flare-ups and easier breathing.
Possible side effects and complications of CHF treatments
Treatments for CHF, while essential, can have their own risks. Some of the more common complications include:
- Low blood pressure (hypotension), which can make you feel dizzy or lightheaded,
- Kidney issues, especially if medications affect fluid or salt balance,
- Increased risk of infections, particularly if frequent hospital stays or intravenous lines (central IVs) are needed.
It’s not about scaring you, but about being real: every medication and therapy comes with trade-offs. Monitoring for these potential side effects is part of why regular follow-up matters.
Treatment options for heart failure with preserved ejection fraction (HFpEF)
When it comes to heart failure with preserved ejection fraction (also called “HFpEF”), treatment is all about addressing both the underlying causes and the symptoms.
For starters, most of the strategies used for earlier stages of heart disease still apply—think blood pressure control, cholesterol management, and generally reducing strain on the heart.
But with HFpEF, there’s extra focus on managing other medical conditions that can tip the balance or worsen symptoms, such as:
- high blood pressure,
- atrial fibrillation (irregular heartbeat),
- diabetes,
- obesity,
- chronic lung disease,
- anemia,
- thyroid problems,
- and kidney issues.
Medications often play a central role. Diuretics (the classic “water pill”) are commonly used to help reduce symptoms like swelling and breathlessness, though they’re mainly for relief—not a cure.
One key thing with HFpEF: learning to juggle and manage multiple health problems really matters. Keeping chronic conditions like diabetes or high blood pressure under control can make a big difference in day-to-day symptoms and the risk of hospitalizations.
Treating the driver
If high blood pressure is contributing, controlling it matters. If coronary disease is involved, that matters. If a rhythm problem is involved, that matters. CHF management is often about finding and treating the underlying reason, not only chasing symptoms.
But there’s more you can do for yourself right now — and it’s not all about prescriptions. While you can’t change your age, family history, or genetics, you can change some daily habits to help lower your risk and support any treatment plan.
A few high-impact steps:
- Stay at a healthy weight for you. Even modest weight loss can ease strain on the heart and lower blood pressure.
- Eat foods that are good for your heart. Think more vegetables, fiber, lean proteins, and less salt and ultra-processed fare.
- Keep moving. Regular activity helps the heart, lungs, and mood — and doesn’t have to mean running marathons.
- Manage stress where you can. Chronic stress hormones can worsen heart issues, so anything from a daily walk to meditation counts.
- Skip tobacco and recreational drugs — and if you drink alcohol, consider cutting back or stopping.
- Stay on top of your other health conditions. Managing diabetes, high blood pressure, and cholesterol all work in your favor.
None of these are magic fixes, but they’re part of treating the whole picture — not just the numbers or symptoms. Small steps add up, and your heart will thank you.
Treatment Options by Stage: What Actually Changes?
You might have seen CHF divided into stages (A through D), which helps guide what treatment makes sense at each point. Let’s break down what typically happens as CHF progresses:
Early-Stage (Stage A): Risk Reduction
At this point, we’re really talking about folks at risk—maybe you have high blood pressure, diabetes, or a family history, but no real heart failure symptoms (yet).
Here’s what’s usually recommended:
- Regular movement—think daily walks, not ultramarathons.
- Avoiding tobacco in all its forms.
- Managing blood pressure and cholesterol with lifestyle tweaks and, if needed, medication.
- Limiting or skipping alcohol and recreational drugs.
- In some cases, starting meds like ACE inhibitors or ARBs if you have additional risk factors. These can help protect the heart even before symptoms show up.
Middle Stages (Stage B): Extra Protection
Now, maybe there’s evidence the heart isn’t pumping quite right (like a lower ejection fraction), but you haven’t started noticing symptoms. The focus is on keeping things stable:
- All the healthy habits from earlier.
- Medications like ACE inhibitors, ARBs, or beta blockers—especially if your heart’s pumping power is reduced, or you’ve had a heart attack.
- Sometimes additional meds, like aldosterone antagonists, if tests show they could help.
- Occasionally, procedures to address trouble spots like blocked arteries or faulty valves, if those are the drivers here.
Symptomatic Stages (Stage C): Symptom Relief and Stability
Now we’re dealing with noticeable symptoms—shortness of breath, swelling, fatigue.
The game plan might include:
- Diuretics (“water pills”) to help shed extra fluid and ease congestion.
- Meds to support heart function—beta blockers, aldosterone antagonists, sometimes newer options like SGLT2 inhibitors.
- Tailoring additional meds to your background and symptoms. For example, certain combinations may be more helpful for specific populations.
- Tracking weight daily (let your provider know if you gain or lose several pounds unexpectedly).
- Limiting salt in your diet and sometimes restricting fluids.
- Considering advanced therapies—like a special pacemaker (to coordinate heart beats) or an internal defibrillator (ICD) if your risk for dangerous rhythms is high.
The goal here: keep you feeling better and out of the hospital, while slowing progression.
Advanced Stage (Stage D): When Symptoms Persist
Some people reach a point where symptoms are tough to control, even with the above treatments.
At this stage, it’s a team effort—exploring:
- More intensive medications (sometimes delivered by IV).
- Considering advanced support devices to help the heart pump, or even a heart transplant for some.
- Focusing on comfort—involving palliative or hospice care for quality of life, if appropriate.
Heart Failure with Preserved Pumping (HFpEF)
Here, the issue isn’t weak pumping, but the heart not relaxing or filling well—often with many other medical issues along for the ride. Treatment usually means:
- All the lifestyle and risk-reduction steps from earlier stages.
- Targeting underlying problems—blood pressure, atrial fibrillation, diabetes, obesity, kidney or lung disease.
- Diuretics to control fluid and relieve symptoms.
Big takeaway: Managing other health issues—like diabetes, kidney disease, anemia, thyroid, or lung problems—matters just as much as heart medications for staying stable.
Treating CHF is about more than just “taking a pill for your heart.” It’s about stacking small advantages, removing triggers, and making changes that fit into your life long-term.
What’s safe advice (and what isn’t)
It’s reasonable to do the basics:
- take symptoms seriously,
- don’t ignore breathing changes,
- keep follow-up with your clinician if you’ve been diagnosed.
Self-care matters. Beyond those basics, managing congestive heart failure (CHF) day-to-day means sticking with your medications, making time for safe activity, following a low-sodium diet, and keeping track of any new or worsening symptoms. If you notice changes, let your provider know promptly—don’t wait for things to spiral.
Stay connected with your care team by keeping regular appointments. CHF is a chronic condition that can sometimes change quickly, so having a plan and being proactive matters.
Thinking ahead: It’s also wise to talk with loved ones and your provider about your care preferences, especially if you’re dealing with CHF as an ongoing issue. Consider putting your wishes in writing—like an advance directive or living will—while you’re well and able to make decisions calmly. This can help ensure that, should anything change suddenly, your priorities are clear to everyone involved.
What we don’t want you doing is:
- stopping or starting medications on your own,
- using online “cure” advice,
- assuming swelling or breathlessness is “just getting older.”
If symptoms are changing quickly, that’s not the moment for internet medicine — it’s the moment for evaluation.
What are the possible complications of congestive heart failure?
CHF doesn’t just affect the heart—it can ripple out to impact many other parts of the body. Here are some of the more common complications we watch for:
- Abnormal heart rhythms (arrhythmias), which can make symptoms worse or even be life-threatening in some cases.
- Sudden cardiac arrest—rare, but serious—if the heart’s rhythm becomes dangerously unstable.
- Problems with your heart valves, as extra fluid can cause the valves to leak or struggle to keep up.
- Fluid buildup in the lungs (pulmonary edema), making breathing even harder and sometimes requiring urgent care.
- Increased pressure in the lungs (pulmonary hypertension), which can stress the heart’s right side over time.
- Kidney challenges, since lower blood flow to the kidneys can affect how well they filter fluids and waste.
- Liver congestion or damage, often from backed-up blood flow.
- Nutritional concerns, including trouble maintaining a healthy weight or getting enough nutrients, especially in more advanced stages.
It’s a lot—but knowing the possible roadblocks helps us keep a closer eye on things and act early if something changes.
Advance directives: A gift for your future self (and everyone else)
It’s not the most exciting topic at a dinner party, but if you’re living with CHF, making decisions about your care before a crisis hits is one of the most compassionate things you can do—for both yourself and the people who love you.
Why does this matter? CHF is a condition that can change speed faster than the weather in Chicago. In a calm moment, you can think through what treatments and interventions fit your goals and values. Writing down your preferences in an advance directive or living will isn’t about giving up—it’s about making sure your wishes are respected if there comes a time when you can’t voice them yourself.
A few reasons to consider preparing one sooner rather than later:
- It spares your family the agony of guessing your wishes in stressful situations.
- It helps your medical team align your care with what matters most to you.
- It’s a lot easier to think clearly and make thoughtful decisions when you’re feeling well (not in the middle of an emergency room whirlwind).
Need a starting point? Most states have easy-to-use forms, and organizations like the National Hospice and Palliative Care Organization (https://www.nhpco.org/) offer resources to walk you through the process.
Having your choices written down doesn’t mean you have to stick to them forever. You can revisit and update them as your health and priorities evolve. It’s just one more way to stay in the driver’s seat with your health—rain or shine.
Warning symptoms that shouldn’t wait
If you’re dealing with possible CHF symptoms (or you already have CHF), these are warning symptoms that shouldn’t wait:
- Severe or rapidly worsening shortness of breath, especially at rest
- New or worsening chest pain, pressure, or tightness
- Fainting, near-fainting, severe weakness, or new confusion
- Bluish lips/face or obvious breathing distress
- A very fast or irregular heartbeat with feeling unwell
- Symptoms that are escalating quickly or feel different from your normal baseline
We’d rather you get checked and it turns out to be manageable than wait until you’re in a worse spot.
If you’re experiencing shortness of breath, chest discomfort, new swelling, or symptoms that feel like they’re getting worse — and you’re in or near Angleton or elsewhere in Brazoria County — it’s reasonable to get evaluated. Angleton ER is open 24/7 with board-certified physicians and on-site diagnostics, including lab testing and imaging such as CT, X-ray, and ultrasound, when needed.
Educational only. This is not medical advice or a diagnosis. If symptoms are severe, rapidly worsening, or you’re concerned, seek in-person evaluation.
Frequently Asked Questions
What is congestive heart failure (CHF)?
Congestive heart failure means the heart isn’t keeping up with the body’s needs the way it should, and the body may hold onto fluid that can back up into the lungs or cause swelling. It does not mean the heart has stopped.
What causes congestive heart failure?
Common causes include long-term strain (like uncontrolled high blood pressure), damage to the heart muscle (including reduced blood flow to the heart), rhythm problems, and triggers like infections or medication changes that worsen symptoms.
What are the symptoms of congestive heart failure?
Many people notice shortness of breath, reduced stamina, swelling in the legs/ankles, unusual fatigue, and sometimes cough or a congested feeling in the chest.
How is congestive heart failure diagnosed?
Diagnosis typically involves your symptom history, a physical exam, and tests like an EKG, blood tests, and imaging. A heart ultrasound (echocardiogram) is often used to better understand how the heart is functioning.
Is congestive heart failure curable?
CHF is usually managed rather than “cured” in the way people hope the word means. Many people do improve significantly with the right treatment plan and by addressing the underlying cause — but it’s important to avoid internet promises and work with a clinician.
When should someone with CHF go to the ER?
If symptoms are severe, rapidly worsening, or include warning symptoms that shouldn’t wait (like chest pain, severe shortness of breath, fainting, bluish lips/face, or feeling seriously unwell), urgent evaluation is appropriate