Colitis is an inflammation of the colon and can emerge in diverse forms. Some types of colitis may result in a life-threatening condition, so it is vital to diagnose the type of colitis affecting you since treatment varies for each.
Collagenous colitis is a rare type of bowel inflammation affecting the colon and is characterized by persistent non-bloody diarrhea and abdominal pain or cramps. Adults aged 50 and above are more likely to develop this condition than other age groups.
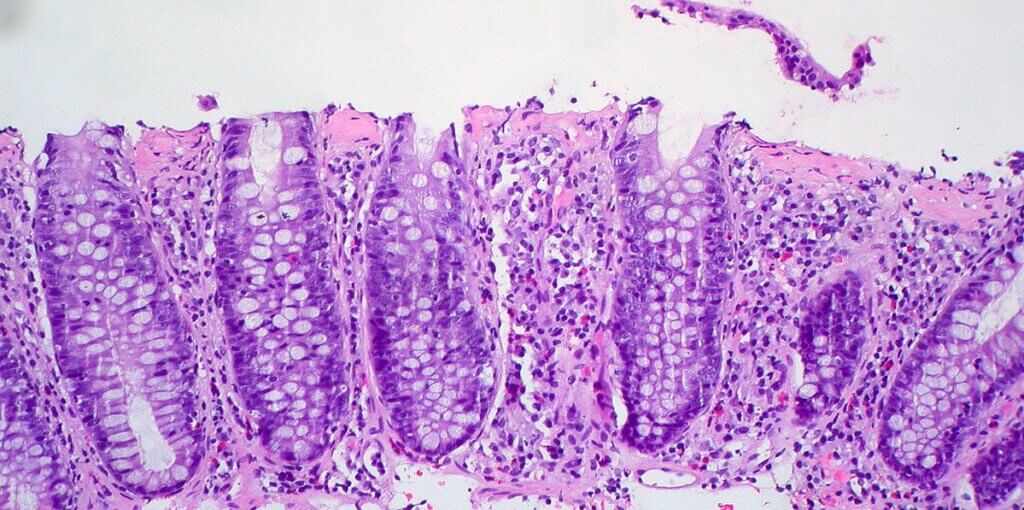
This condition belongs to a group known as microscopic colitis, so called because the inflammation isn’t visible on the surface of the colon during a colonoscopy or sigmoidoscopy—it only shows up when a tissue sample (biopsy) is examined under a microscope. In collagenous colitis, the middle layer of the colon lining—made up of collagen, a protein your body uses for building connective tissues—becomes abnormally thickened and swollen. This excess layer of collagen is what distinguishes collagenous colitis from other types of colitis, but it can only be detected microscopically.
Researchers categorize collagenous colitis as one of the two types of microscopic colitis because inflammation on the outer surface of the colon is not visible when examined through a colonoscopy or sigmoidoscopy. But visible when a biopsy goes under a microscope.
Cause of Collagenous Colitis
While researchers are still unsure of the exact cause of collagenous colitis, several studies have shown that collagenous colitis can be caused by genetic and environmental factors.
It also occurs when the immune system attacks bacteria in the colon.
Several pieces of research suggest that the intake of certain medications such as proton pump inhibitors and Nonsteroidal anti-inflammatory drugs (NSAIDs) can trigger the development of collagenous colitis. However, there is no consistent data to support this claim.
Researchers also suggest that women are more likely to be affected by this disease than men. An elevated estrogen level in women contributes to the high disparity between both genders.
While gluten, a protein found in products like wheat, oat, and barley, is not the actual cause of microscopic colitis, it could trigger the inflammation of the colon.
Other Possible Triggers and Risk Factors
Although the precise cause remains elusive, some theories suggest that collagenous colitis may be a type of autoimmune response—meaning the immune system mistakenly produces inflammation, acting as if the colon is infected or injured, even when it isn’t. Other possible triggers and risk factors include:
- Infections: Certain infections that damage the colon lining, such as those caused by Clostridioides difficile or Yersinia bacteria, may play a role.
- Medications: Regular use of drugs like NSAIDs, proton pump inhibitors (PPIs), and selective serotonin reuptake inhibitors (SSRIs) has been linked to a higher risk, possibly due to their impact on the colon’s immune defense.
- Allergens: Allergens in the colon, including certain foods and environmental factors like pollen, may contribute to inflammation in susceptible individuals.
Who Is at Greater Risk?
You may be more likely to develop collagenous colitis if you:
- Are female (the condition is roughly three times more common in women than men)
- Have a family history of inflammatory bowel disease or other gastrointestinal conditions such as celiac disease, irritable bowel syndrome (IBS), or bile acid malabsorption (BAM)
- Have a systemic autoimmune disease, such as rheumatoid arthritis or scleroderma
- Smoke—studies indicate that smoking can increase your risk significantly
While ongoing research aims to clarify these connections, being aware of these risk factors can help you and your healthcare provider identify and manage symptoms more effectively.
Symptoms of Collagenous Colitis
It is common for collagenous colitis patients to experience diarrhea and abdominal pain; however, the severity and duration vary according to each individual.
You may experience mild discomfort, while a loved one may experience disabling symptoms. Other symptoms of collagenous colitis include:
- The feeling of bowel movement
- Inflammation, infection, chills, and fever.
- Constant pain
- Abdominal pain occurring in waves
- Bloating
- Flatulence
Collagenous and lymphocytic cases that do not respond to medication may require surgery to remove all or part of the colon.
Diagnosis
Diagnosis is the first step to treating collagenous colitis. A gastroenterologist will perform a physical examination and ask questions about your lifestyle habits, medical history, medication, and eating patterns.
For an accurate diagnosis, your doctor will take different biopsies from a separate section of your colon to examine under a microscope.
When in doubt, your doctor may order additional tests such as CT scans, MRIs, blood and stool tests to ascertain if another underlying gastrointestinal condition causes your condition.
Treatment
To treat microscopic colitis, the first thing you should do is change your diet. Your doctor may advise you to eat low-fat food and avoid foods rich in gluten to help relieve diarrhea.
Your doctor may introduce good bacteria known as lactobacilli to replace immunogenic strains of bacteria that may be responsible for collagenous colitis.
Your doctor may prescribe antidiarrheal medication such as loperamide (Imodium) or bismuth subsalicylate (Pepto-Bismol) to reduce discomfort. Your doctor may discontinue the use of medicine as a treatment option if your symptoms persist or worsen.
Can Collagenous Colitis Go Into Remission?
Yes, collagenous colitis can go into remission for many individuals. With an accurate diagnosis and the right treatment plan, you may notice your symptoms improving significantly—or even disappearing entirely for periods of time. However, it’s important to remember that symptoms might return on occasion. Some people require medication intermittently or over the long term, depending on how their body responds. Regular checkups with your healthcare provider can help manage flare-ups and maintain remission.
Surgery
In severe cases, medications may not effectively treat collagenous colitis; your doctor may suggest surgery to remove all or part of your color. However, surgery may not be necessary for collagenous colitis.
Home Remedies
If you experience collagenous colitis, drinking excess water is key to curing this condition. With each bowel movement, you may lose a significant amount of fluid. So adequate fluid intake is crucial to maintaining balance, or it may lead to dehydration, abdominal pain, and cramping.
Eat easily digestible food such as rice, applesauce, and vegetables. Avoid beverages rich in sugar, alcohol, and caffeine that may trigger colitis. You can slowly add fiber back to your diet if symptoms improve.
Avoid spicy food, fried and fatty food. Consistently eating small meals instead of one large meal may help heal faster and relieve diarrhea.
While the risk of death or developing colon cancer is relatively low with collagenous colitis, your doctor may test for other conditions with the symptoms you are experiencing if your state doesn’t improve after exhausted all options. Always remember that eating healthy is the key to living your best life.
Outlook and Living Well with Collagenous Colitis
With the right diagnosis and treatment, most people find significant relief from the symptoms of collagenous colitis. For some, the disease can go into remission, with symptoms disappearing for long stretches. Others may notice their symptoms flare up occasionally, requiring on-and-off medication or adjustments to their treatment plan.
Don’t be discouraged if you find yourself needing to try different medications or dietary changes before finding what works best for you. Living with a chronic condition can be challenging, but many people experience a noticeable improvement in their quality of life once the correct diagnosis is made and a personalized treatment approach is in place.
Remember, small changes—like staying hydrated, managing stress, and making thoughtful food choices—can go a long way in managing your symptoms and supporting your overall well-being.