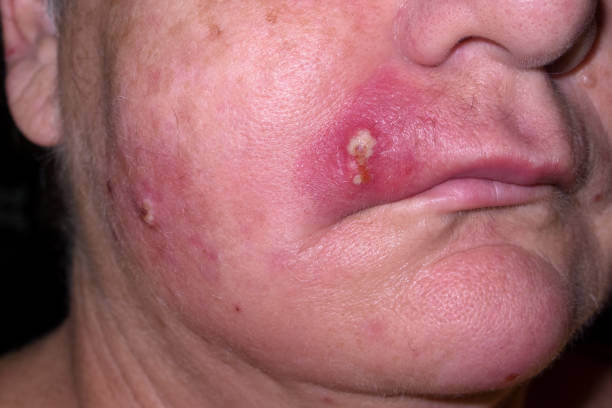
Did you know that Staph bacteria can hibernate on your skin surface and, in this environment, can be relatively harmless? However, if you have an injury or a weak immune system, these harmless bacteria infiltrate the skin and cause an infection.
Who’s at Risk?
While anyone can get a staph infection, some people are more likely to have trouble with these sneaky microbes. Your risk increases with age, and if you have a weakened immune system, staph can become a bigger concern. People managing chronic skin conditions, like eczema, or those with open wounds, burns, or recent surgery, are also easier targets.
Other factors that can make you more susceptible include:
- Living with diabetes, kidney failure, or HIV
- Undergoing chemotherapy or taking systemic steroids
- Having medical devices inside the body (like artificial joints or catheters)
- Using dialysis
- Experiencing frequent skin injuries, injections, or even acupuncture
Living Situations and Activities That Raise Risk
Crowded environments—think college dorms, nursing homes, military barracks, or shelters—are prime real estate for staph to spread. Athletes in contact sports, such as football or wrestling, and people who work closely with animals (like farmers and veterinarians) also have an increased risk, as do those who use injected illicit drugs or manage chronic skin disorders.
Some groups, such as young children, older adults, and certain ethnic populations, may experience higher rates of certain staph infections.
And here’s the kicker: some strains, like MRSA (methicillin-resistant Staphylococcus aureus), shrug off standard antibiotics, making prevention and early treatment even more important.
Staphylococcus infections are responsible for causing different illnesses such as boils, acne, impetigo, or carbuncles. While most of these infections are non-life-threatening, staph can cause severe illness or death if it enters the bloodstream.
Treatment usually involves antibiotics; however, some strains no longer respond to antibiotics.
What are the Primary types of Staph Bacteria?
Staph bacteria contains at least 30 different strains that can affect humans; here are the primary strains of staph bacteria. You must understand the various strains of staph bacteria to provide the best treatment properly.
Staphylococcus Aureus
Skin bacteria such as Staphylococcus aureus are pretty common and affect about 20% – 30% of Americans. Staph can colonize on all parts dot the skin; however, they are primarily found in the nose, hands, and perineum (between the thighs).
Staphylococcus aureus causes mild skin and tissue irritation such as acne, cellulitis, furuncles, and abscess (boil). Although most staph infections are not severe, they can progress into life-threatening conditions if not properly managed.
Often, staph infections begin as small red bumps on the skin, which may quickly develop into deep, painful abscesses. As the infection spreads, you might notice changes such as:
- Discolored skin—appearing red, purple, or brown depending on your skin tone
- Swelling, warmth, and tenderness around the affected area
- Hardness under the skin
- Blisters that may break open, leaving a raw, burn-like surface
- Fever and chills
- A general sense of feeling unwell (malaise)
- Significant pain
These symptoms can signal a more serious infection, including conditions like cellulitis, mastitis, necrotizing fasciitis, or staphylococcal scalded skin syndrome. Early recognition and treatment are key to preventing complications and ensuring a full recovery.
Methicillin-resistant Staphylococcus aureus (MRSA)
Methicillin-resistant Staphylococcus aureus (MRSA) is a virulent and drug-resistant strain of Staph bacteria. Research shows that MRSA mutates due to antibiotics overuse, making it resistant and challenging to treat using conventional antibiotics.
MRSA infections often begin as small red bumps on the skin, which can quickly develop into deep, painful abscesses. These abscesses may require professional medical drainage and can be mistaken for spider bites or other skin problems at first. Because MRSA is resistant to many standard antibiotics, it can spread rapidly and is more difficult to manage than typical staph infections.
Around 1% of the 20%-30% of Americans who carry staph colonize this strain. Without proper management, MRSA may cause life-threatening conditions or even death.
VRSA (Vancomycin-resistant S. aureus)
VRSA, also known as GISA (glycopeptide intermediate Staphylococcus aureus), is a rare strain of staphylococcus that has developed resistance to a class of glycopeptide antibiotics called vancomycin.
Treatment for this strain of staph infection is limited because doctors only recommend vancomycin as a last resort when another form of medication fails.
If you suspect a staph infection, contact your doctor to administer a culture for diagnosis and treatment.
How do you contract Staph Infection?
Knowing the causes and modes of transmission of the staph bacteria is the best way to deal with and prevent its spread. We’ve listed some of the most common reasons below.
Participation in Contact Sports
Engaging in contact sports—such as wrestling, football, or mixed martial arts—significantly increases your risk of contracting a staph infection. The frequent skin-to-skin contact, as well as the likelihood of small cuts, scrapes, or bruises during play, creates easy entry points for bacteria.
Moreover, athletes often share personal items like towels, razors, water bottles, gym equipment, and team uniforms, which can further promote the spread of staph bacteria. Locker rooms and gym facilities, if not cleaned properly, provide an environment where these bacteria can thrive. Practicing good hygiene—such as showering immediately after training, keeping wounds covered, and not sharing personal items—is vital for minimizing the risk of infection.
Skin Penetration
Staph bacteria can be lying dormant on your skin; however, this dormancy can be broken and lead to an active infection if you have an injury or cut.
Ingesting Contaminated Food and Drinks
Staph bacteria can survive in food that has not been stored or prepared correctly. Keeping food at an inappropriate temperature will provide a conducive environment for staph multiplication. Food products that can colonize staph bacteria include fish, milk, mayonnaise, etc.
Importance of Handwashing Before Handling Food
Washing your hands thoroughly before preparing or handling food is a simple but crucial step in preventing the spread of staph bacteria. Our hands frequently come into contact with surfaces and objects that can harbor these microbes, and if you skip handwashing, you risk transferring bacteria directly onto food items.
This is especially important when dealing with items like fish, milk, or mayonnaise, which are more susceptible to bacterial growth. Good hand hygiene significantly reduces the chances of staph contamination, helping keep you and your loved ones safe from potential foodborne illnesses.
Proper Cleaning of Cutting Boards and Counters
To maintain food safety and keep those pesky staph bacteria at bay, always scrub your cutting boards and kitchen counters thoroughly after use. Use warm water and dish soap, making sure to reach into any grooves or crevices where bacteria might hide. After washing, rinse well and allow surfaces to air dry.
For added protection, especially after handling raw meat, consider disinfecting with a diluted bleach solution or white vinegar. This extra step ensures you’re tackling both visible mess and invisible germs, giving staph bacteria one less place to lurk.
Proper Storage of Leftovers
To prevent staph bacteria from multiplying in your food, it’s essential to refrigerate leftovers promptly. Aim to refrigerate any perishable foods within two hours of cooking or serving. In warmer climates or during the summer months—think backyard barbecues or picnics—it’s best to refrigerate within just one hour. Taking this precaution helps keep your meals safe and minimizes the risk of foodborne infection.
Proper Temperature for Cold Food Storage
To keep cold foods safe from staph growth, ensure they are stored at temperatures no higher than 40°F (4°C). Refrigeration at or below this temperature slows bacterial multiplication and helps prevent foodborne infections. Always check that your refrigerator is set to this standard to reduce the risk of staph contamination.
Keeping Hot Foods Safe During Serving
To prevent staph bacteria from multiplying in your food, always serve hot dishes while maintaining a temperature above 140°F (60°C). Use warming trays, slow cookers, or chafing dishes to keep food piping hot if it needs to sit out for any period. This simple precaution goes a long way in reducing the risk of foodborne staph infection.
Use of High Absorbent Tampons
Absorbent tampons can be a suitable breeding ground for staph bacteria due to the wet environment created by the tampon. This type of staph infection can cause toxic shock syndrome (TSS).
Safe Tampon Practices to Prevent Toxic Shock Syndrome
If you use tampons, there are a few important steps you can take to minimize your risk of developing toxic shock syndrome from a staph infection. Start by choosing the lowest absorbency tampon necessary for your flow, as high-absorbency tampons can create a favorable environment for bacteria. Always wash your hands thoroughly before and after inserting or removing a tampon, and remember to change it at least every eight hours—never leave one in for an entire day.
When possible, consider alternating between tampons and pads, especially overnight, to give your body a break and reduce the chances of bacterial buildup. Consistently following these habits can go a long way in keeping you safe from staph-related complications.
What are the Symptoms of Staph Infection?
Generally, staph doesn’t usually cause severe symptoms as long as they are dealt with early; however, you will experience varying symptoms depending on the location and type of infection.
Symptoms for Skin Infection
Staph infections on the skin cause boil that are red and painful acne. They can also cause cellulitis and impetigo.
Symptoms for Septic Arthritis
Staph bacteria can sometimes invade the joints—whether your own or artificial ones—leading to a condition called septic arthritis. This infection most commonly affects larger joints like the knees, but the hips, shoulders, fingers, or toes can also be targets.
Signs that you may be dealing with septic arthritis include:
- Noticeable swelling and redness around the affected joint
- Intense joint pain, especially with movement
- Fever or chills accompanying the joint symptoms
If you suddenly experience joint pain and swelling paired with a fever, it’s essential to see your doctor promptly. Quick intervention can help protect the joint and limit further complications.
Symptoms for Toxic Shock
Toxic shock is a life-threatening condition linked to some strains of bacteria caused by specific surgical procedures or wounds. Toxic shock syndrome can cause:
- Vomiting and diarrhea
- Rask on the skin resembling a sunburn
- High fever
- Abdominal pain
- Muscle ache
Symptoms for Bloodstream Infection (Bacteremia)
When staph bacteria manage to infiltrate your bloodstream, the body can react quite dramatically—and not in a way anyone would welcome. Bloodstream infections, also called bacteremia, are particularly serious since they run the risk of triggering sepsis, a dangerous, system-wide immune response that can progress to organ failure if left untreated.
Typical symptoms you might notice with staph bacteremia include:
- High fever or recurrent chills
- Rapid, shallow breathing or shortness of breath
- Accelerated heart rate
- Sudden confusion, agitation, or feeling disoriented
- Cold, sweaty, or clammy skin
- Intense or worsening pain throughout the body
Recognizing these warning signs early is crucial; without proper prompt treatment, bacteremia can quickly become life-threatening.
Symptoms for Food Poisoning
Staph infection is one of the common causes of food positioning occurring when you ingest contaminated food. Symptoms often resolve within a few days without treatment; however, your doctor may prescribe a few medications to help ease discomfort. In most cases, the symptoms develop rapidly—typically within hours of eating the contaminated food. While staph-related food poisoning tends to come on quickly, the good news is that it usually passes just as fast, often disappearing within a day. Fever is uncommon with this type of food poisoning, so most people recover with rest and proper hydration.
Symptoms of food poisoning include:
- Nausea and vomiting
- Fever
- Dehydration
- Diarrhea
Emergency Symptoms of Sepsis or Septic Shock from Staph Infections
Staph infections, when left unchecked, can sometimes progress into serious conditions like sepsis or septic shock—a true medical emergency. It’s crucial to recognize these warning signs and act quickly. If you experience any of the following symptoms, seek emergency medical attention without delay:
- A sudden high fever or uncontrollable chills
- Rapid or shallow breathing, or feeling like you can’t catch your breath
- New or worsening confusion, disorientation, or difficulty staying alert
- Cool or clammy skin, or skin that appears sweaty and pale
- A rash that spreads quickly or appears in distinct patterns—particularly those resembling the outline of underwear
- Intense pain, either widespread or located in a specific joint or area
- Severe stomach pain, persistent nausea, or vomiting
- Prominent muscle aches or joint swelling
- Ongoing diarrhea not resolving with time
If these symptoms appear—particularly in combination—do not wait. Quick intervention can make all the difference, as sepsis and septic shock can escalate rapidly.
How Can You Prevent Staph Infection?
There are specific preventive measures you can maintain, to keep you and your loved one safe from this infection. Here are the preventive measures to avoid staph infection:
- Practice good hygiene such as washing your hands with soap and water
- Avoid sharing toiletries and sharp personal equipment
- Carefully treats injuries in case of an accident
If you get a minor cut, scrape, or wound, make sure to wash your hands first, then gently clean the affected area with soap and water. Cover the injury with a dry, clean bandage to keep out bacteria and prevent infection. For deeper or more serious wounds, seek medical attention promptly.
While your skin heals, avoid soaking the area in pools, hot tubs, or natural bodies of water like lakes, as these can harbor bacteria. And remember—not picking at scabs or wounds helps them heal faster and reduces your risk of developing a staph infection.
- Practice food hygiene and store food at a temperature of 280F -320F. In addition, always wash your hands thoroughly before handling any food, and make sure to clean cutting boards and countertops with soap and water after use. If food will be sitting out, keep hot foods hot (above 140°F/60°C) and cold foods cold (at or below 40°F/4.4°C). Refrigerate leftovers as soon as possible to prevent bacteria from multiplying.
Cleaning Practices to Prevent Staph Spread
To help keep staph bacteria at bay, make cleaning your personal and shared spaces a regular habit. Frequently touched items—think keyboards, TV remotes, light switches, gym equipment, and locker handles—can quietly harbor bacteria just waiting for an opportunity to spread. Give these surfaces a wipe-down with a disinfectant that’s proven to kill staph; be sure to follow the product’s directions for safe and effective use.
When it comes to laundry, there’s no need to go overboard with harsh chemicals. Standard laundry detergents are usually enough. Wash your clothes, towels, and bedding according to the care instructions, using warm or hot water when possible. This not only helps remove staph bacteria but also keeps your fabrics fresh.
Taking these cleaning steps, combined with diligent hygiene, goes a long way in protecting yourself and those around you from staph infections.
If you experience early symptoms of an active staph infection, consult your doctor for diagnosis and treatment.
How do you Treat Staph Infection?
Your doctor will recommend a treatment course depending on the type of infection. If you have an abscess, your doctor may drain the puss or prescribe medications to relieve pain and discomfort.
In cases of antibiotic-resistant strains of staph bacteria, consult your doctor about alternative treatment options.